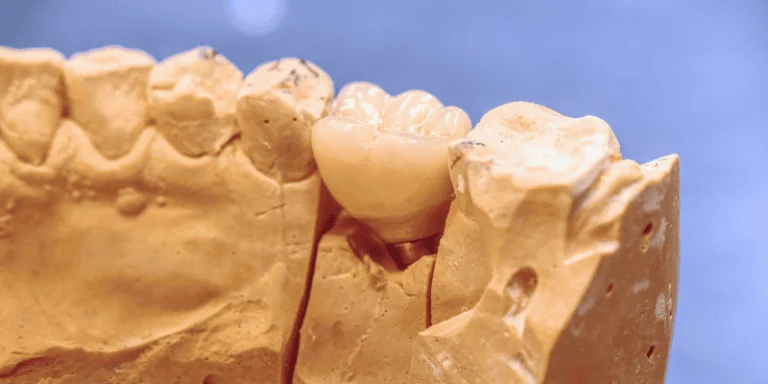
Dental implants are a major investment in your smile, so you naturally want to know how long they’ll last before committing to the procedure.
Most dental implants last 10 to 30 years with proper care, and studies show a 90-95% success rate over 10 years.
The implant post itself is designed to be permanent since it fuses with your jawbone, but the crown on top may need replacement after 15 to 20 years due to normal wear.
Several factors determine whether your implants will last decades or fail within just a few years. Your oral hygiene habits, bone health, lifestyle choices, and even the skill of your surgeon all play important roles.
Understanding how long dental implants last and what can shorten their lifespan helps you protect your investment and keep your smile looking great.
Key Takeaways
- Dental implants typically last 10 to 30 years, with success rates of 90 to 95 percent over a decade when properly maintained
- Poor oral hygiene, smoking, teeth grinding, insufficient bone, and certain medical conditions can cause implants to fail early
- Good daily brushing and flossing, regular dental checkups, avoiding smoking, and protecting against teeth grinding extend implant lifespan significantly
How Long Dental Implants Really Last
Dental implants can last 15 to 25 years or even a lifetime with proper care, though different parts wear at different rates. The metal post typically outlasts the crown, which may need replacement after 10 to 15 years.
Typical Lifespan of Implant Post
The implant post is the titanium screw that sits in your jawbone and acts as an artificial tooth root. This component can last 25 years or more, and many patients keep their posts for life.
Implant posts typically last 20 to 30 years because titanium bonds directly to your bone through a process called osseointegration. Once this bond forms, the post becomes stable and permanent.
The post’s longevity depends on your bone density and overall health. People with strong, healthy jawbones see better results than those with bone loss or conditions like osteoporosis. Your body accepts titanium as if it were natural tissue, which is why these posts rarely fail once they’re fully integrated.
Crown and Abutment Replacement Timelines
Your crown is the visible tooth-colored part that attaches to the implant post through a connector called an abutment. Crowns usually last 10 to 15 years before needing replacement.
The crown wears down faster than the post because it handles all your chewing forces. Materials like porcelain or ceramic can chip or stain over time, especially if you grind your teeth or eat hard foods regularly.
The abutment typically lasts as long as the crown and may be replaced at the same time. Some dentists recommend replacing both pieces together to ensure a proper fit. Your back teeth experience more pressure than front teeth, so crowns on molars may wear out faster than those in the front of your mouth.
Success Rates and Longevity Statistics

Dental implants have a 95 to 98 percent success rate at the 10-year mark. Research shows that 96.8 percent of implants survive at 10 years and 94 percent last 15 years.
These high success rates make dental implants the most reliable tooth replacement option available. Even after 20 years, studies show survival rates between 90 and 95 percent for well-maintained cases.
Early failures usually happen within the first year due to poor bone integration or infection. Late failures occur years later and often result from gum disease around the implant or excessive force from teeth grinding.
Your chances of long-term success improve significantly when you maintain good oral hygiene and attend regular dental checkups.
What Affects Dental Implant Longevity
Several key factors determine whether your dental implants will last decades or fail early. Your daily habits, overall health, and the skill of your dental team all play major roles in how long your implants stay functional.
Oral Hygiene and Maintenance
Your daily cleaning routine directly impacts how long your implants survive. Brushing twice a day and flossing around your implants removes plaque that can cause infections.
When plaque builds up around implants, it leads to peri-implantitis. This infection damages the gum tissue and bone supporting your implant. Peri-implantitis is a leading cause of implant failure if left untreated.
Professional cleanings every six months help catch problems early. Your dentist can remove hardened plaque you can’t reach at home. Regular checkups let your dental team monitor your bone density and gum health around the implant.
Poor oral hygiene makes your implants more likely to fail within the first few years. The good news is that proper care helps most implants last 10 years or longer with success rates between 90 and 95 percent.
Curious how long your dental implants could last based on your health and habits? Complete your registration paperwork before your appointment to get a personalized treatment plan discussion.
Lifestyle and Medical Factors
Smoking significantly reduces your implant success rate. Studies show implant failure rates of 11 percent in smokers compared to just 5 percent in nonsmokers. Smoking restricts blood flow to your jawbone, which slows healing and weakens the bond between the implant and the bone.
Certain medical conditions affect your implants, too. Diabetes, osteoporosis, and weakened immune systems can interfere with healing. These conditions may also cause bone loss around your implant over time.
Teeth grinding puts excessive force on your implants. This pressure can loosen the implant or crack the crown attached to it. A night guard protects your investment if you grind your teeth.
Some medications can affect implant success. Blood thinners and immunosuppressive drugs can affect healing. Radiation therapy to the head or neck area may also impact your jawbone health.
Implant Placement and Professional Skill
The experience of your surgeon matters more than you might think. An inexperienced surgeon can cause implant failure through poor placement or by attaching the crown before the implant is stable.
Your jawbone quality determines whether an implant can stay secure. Dentists use X-rays and 3D imaging to check if you have enough bone before implant placement. Insufficient bone means the implant lacks a solid foundation.
Some people need bone grafts before getting implants. This procedure builds up the jawbone to create better support. Your surgeon should thoroughly examine your bone density and plan accordingly.
Proper implant positioning prevents future problems. The implant must be placed at the correct angle and depth in your jawbone. Tissue damage during surgery can also compromise healing and long-term success.
Dental Implant Structure and Osseointegration
A dental implant consists of three distinct parts that work together to replace your missing tooth, and its success depends on a biological process called osseointegration that bonds the implant to your jawbone. The type of implant you receive affects both the procedure and long-term results.
Parts of a Dental Implant
Your dental implant has three main components that create a complete tooth replacement system.
The implant post acts as an artificial tooth root. This small screw-shaped piece is surgically placed into your jawbone. Most posts are made from medical-grade titanium, though some use zirconia ceramic. The post typically measures 3 to 6 millimeters in diameter and 10 to 15 millimeters in length.
The abutment connects the implant post to the visible crown. This small connector piece attaches to the top of the post after your jawbone has healed around it. Your dentist secures the abutment with a tiny screw. It can be made from titanium, zirconia, or gold alloy.
The crown is the visible part that looks like your natural tooth. It’s custom-made to match your other teeth in size, shape, and color. Most crowns are made from porcelain, ceramic, or porcelain fused to metal.
The Role of Osseointegration
Osseointegration is the biological bonding process between your jawbone and the implant post that makes dental implants permanent.
After your dentist places the implant post into your jawbone, your bone cells begin growing around the titanium surface. This process typically takes 3 to 6 months. The bone gradually forms a direct structural connection with the implant material, creating a stable foundation.
Successful osseointegration depends on several factors:
- Adequate bone density and volume at the implant site
- Proper surgical technique and implant placement
- Your overall health and healing ability
- Avoiding pressure on the implant during healing
Your jawbone must fully integrate with the post before the abutment and crown can be attached. Without complete osseointegration, the implant can fail. This is why your dentist waits several months between placing the post and attaching the final crown.
Types of Dental Implants
Different implant types serve different needs based on your bone structure and treatment goals.
Endosteal implants are the most common type. These are the screw-shaped posts placed directly into your jawbone. They work well if you have sufficient bone height and width. Endosteal implants typically last 20 to 30 years with proper care.
Subperiosteal implants sit on top of your jawbone but under your gum tissue. Your dentist might recommend this type if you don’t have enough healthy jawbone for traditional implants and want to avoid bone grafting procedures. These are less common today.
Zygomatic implants anchor into your cheekbone rather than your jawbone. These are the longest implants available and are only used for upper jaw replacements when you have severe bone loss.
| Implant Type | Placement Location | Best For |
| Endosteal | Inside jawbone | Most patients with adequate bone |
| Subperiosteal | On top of jawbone | Limited bone without grafting |
| Zygomatic | Cheekbone | Severe upper jaw bone loss |
Common Reasons Dental Implants Fail Early
Early implant failure happens within the first few months after placement and usually stems from issues with healing, infection, or too much pressure on the new implant. Understanding these risk factors helps you protect your investment and catch problems before they become serious.
Poor Oral Hygiene and Peri-Implantitis
Keeping your mouth clean is one of the most important things you can do for your implant. When you don’t brush and floss regularly, bacteria build up around the implant site and cause peri-implantitis.
Peri-implantitis is an infection that attacks the gum tissue and bone around your implant. It works a lot like gum disease but moves faster and can destroy the bone that holds your implant in place. If left untreated, this infection leads to bone loss and eventually implant failure.
Signs of peri-implantitis include:
- Red or swollen gums around the implant
- Bleeding when you brush or floss
- Bad breath that won’t go away
- Pus around the implant site
You need to brush twice daily and floss around your implant just like you would with natural teeth. Regular dental cleanings every six months help catch early signs of infection before they cause permanent damage.
Health and Lifestyle Risks
Your overall health plays a big role in whether your implant succeeds or fails. Certain medical conditions make it harder for the jawbone to fuse with the implant during the healing period.
Uncontrolled diabetes slows down healing and increases your risk of infection. Osteoporosis weakens your bones and makes it harder for the implant to integrate properly. Smoking is one of the biggest risk factors because it restricts blood flow to your gums and reduces oxygen levels needed for healing.
Health factors that increase implant failure risk:
- Uncontrolled diabetes
- Osteoporosis or bone disorders
- Autoimmune diseases
- Smoking or tobacco use
- Certain medications that affect bone healing
If you smoke, quitting before getting an implant greatly improves your chances of success. Talk to your dentist about managing any health conditions before your procedure.
Bruxism and Excessive Force
Grinding or clenching your teeth puts extreme pressure on your implant before it has time to heal. This condition, called bruxism, can prevent the implant from properly bonding with your jawbone.
Even after your implant has healed, chronic grinding can wear down the implant components and cause it to feel loose. The constant force damages the bone tissue around the implant and shortens its lifespan.
Many people grind their teeth at night without realizing it. Your dentist can fit you with a custom nightguard that protects your implant while you sleep. This simple device distributes the pressure evenly and prevents damage to both your implant and natural teeth.
Not sure if your lifestyle or health conditions could shorten implant life? Talk with our dental professionals to review your risks and learn how to maximize implant longevity.
How to Extend the Lifespan of Your Dental Implants
Your daily habits and preventive care are the biggest factors in how long your implants remain healthy. Simple steps like proper cleaning, protecting against grinding, and keeping regular appointments can add years to your investment.
Daily Cleaning Techniques
You need to clean around your implants every day to prevent gum disease and bone loss. Regular toothpaste and a soft-bristled brush are effective for the crown surface, but you should brush at least twice daily.
The area where your implant meets the gum needs special attention. Use implant-specific floss or interdental brushes to clean under and around the crown. These tools reach spaces regular floss might miss.
A water flosser can help remove food particles and bacteria from hard-to-reach spots. Set it to medium pressure and aim the stream at the gum line around your implant. This works especially well if you have multiple implants or bridges.
Don’t skip your tongue and other natural teeth. Good oral hygiene throughout your mouth reduces bacteria that could affect your implants. Some dentists recommend antimicrobial rinses, but ask before adding one to your routine.
Protective Measures and Night Guards
Grinding or clenching your teeth puts extra force on implant crowns and can cause damage over time. A custom night guard protects both your implants and natural teeth while you sleep.
Your dentist can make a guard that fits your bite exactly. Over-the-counter options exist, but custom guards distribute pressure more evenly and last longer. Wear it every night if you grind your teeth.
Lifestyle changes also protect your implants. Quit smoking if you currently smoke, since it reduces blood flow to your gums and weakens bone. Control conditions like diabetes that affect healing and bone health.
Avoid chewing ice, hard candy, or other very hard foods that could crack your crown. Your implant crown is strong but not indestructible.
Regular Dental Visits
Professional cleanings remove buildup that home care misses. Schedule dental visits every six months, or more often if your dentist recommends it based on your gum health.
Your dentist will check the stability of your implant and look for early signs of problems. X-rays show bone levels around the implant post, helping detect issues before they become serious.
These visits often include measuring gum pocket depths around your implant. Deeper pockets can signal an infection that needs treatment. Catching how to make implants last longer problems early prevents bigger repairs later.
Your dentist may also adjust your bite if needed. Uneven pressure from a high spot can stress your implant over time.
Do Dental Implants Last Forever? Managing Expectations
Dental implants don’t last forever, though many patients keep them for decades with proper care. The crown typically needs replacement before the implant post, and certain warning signs tell you when professional attention is needed.
When Replacement May Be Needed
The implant post itself can last 20 to 30 years, or even a lifetime, when your bone remains healthy and strong. However, the crown attached to the implant usually needs replacement sooner.
Most crowns last 10 to 15 years before wear, staining, or damage necessitate replacement. Your bite force, eating habits, and how well you maintain the crown all affect how long it holds up.
You might need earlier replacement if you:
- Grind your teeth at night without wearing a protective guard
- Chew hard foods like ice or hard candy regularly
- Develop gum disease that weakens the tissues around your implant
- Experience bone loss from medical conditions or poor oral hygiene
The good news is that replacing a crown is much simpler than placing a new implant. Your dentist can usually swap out the crown while keeping the original post intact.
Recognizing Signs of Implant Problems
Watch for changes that signal potential implant failure so you can get help before the problem gets worse. Early treatment protects both your implant and the bone supporting it.
Common warning signs include:
- Swelling or redness in your gums around the implant
- Bleeding when you brush or floss near the implant site
- A loose feeling when you bite down or touch the implant
- Pain or discomfort that doesn’t go away
- Changes in how your bite feels
Contact your dentist right away if you notice any of these symptoms. Regular dental checkups catch problems early, often before you feel any discomfort.
Long-lasting implants start with proper planning and follow-up care. Reach out today at our Minot, ND clinic for a professional evaluation and keep your smile strong for years to come.
Frequently Asked Questions
Dental implants can last decades when conditions are right, but success depends on bone health, daily care habits, and how your body responds to the implant. Most patients want to know what affects durability and what to expect during recovery.
What factors can affect the longevity of dental implants?
Your oral hygiene habits play a major role in how long your implants survive. If you don’t brush twice daily and floss regularly, plaque builds up and can cause gum disease around the implant.
Smoking is another big factor that reduces implant success rates to about 11 percent failure compared to 5 percent in nonsmokers. The chemicals in cigarettes reduce blood flow to your gums, which slows healing and weakens the bond between implant and bone.
Your jawbone quality matters too. You need enough healthy bone to anchor the implant securely. If you have osteoporosis or bone loss from gum disease, your implant may not have a solid foundation.
Teeth grinding can damage implants over time. The constant pressure and movement can loosen the implant or crack the crown attached to it.
Certain health conditions like diabetes, a weakened immune system, or cardiovascular problems can make implant failure more likely. Some medications like blood thinners and immunosuppressive drugs also affect healing.
What is the average success rate of dental implants after 10 years?
Studies show that dental implants have a 90 to 95 percent success rate over 10 years. This means most implants stay firmly in place and function properly for at least a decade.
The high success rate comes from a process called osseointegration. Your jawbone actually fuses with the titanium implant, creating a stable foundation that acts like a natural tooth root.
Are there any common disadvantages associated with dental implants?
The upfront cost is often the biggest drawback for many patients. Dental implants usually cost more than bridges or dentures.
The process takes several months from start to finish. You’ll need time for the implant to bond with your jawbone before the final crown gets attached.
Some people require additional procedures, such as bone grafts, before they can receive an implant. This adds time and expense to the treatment.
There’s always a small risk of complications. Peri-implantitis can develop if bacteria infect the area around your implant, causing inflammation and potential bone loss.
How long can one expect dental implant crowns to maintain their condition?
The crown that sits on top of your implant typically lasts 15 to 20 years before needing replacement. About 50-80 percent of crowns require replacement within this timeframe.
Crowns wear down from normal chewing and biting. They can also chip or crack if you bite something hard or grind your teeth at night.
The good news is that replacing a crown is much simpler than replacing the entire implant. Your dentist can usually put a new crown on your existing implant without surgery.
Can individuals expect to lead a long life with dental implants without complications?
Many people keep their implants for life without any problems. The implant itself is designed to be permanent once it fuses with your jawbone.
Your success depends largely on how well you care for your implants. Regular dental checkups every six months help catch problems early before they become serious.
You need to treat implants as you would natural teeth. Brush them, floss around them, and avoid habits that could damage them.
Some people do experience complications even with good care. Age, health conditions, and medications can all affect how your body responds to the implant over time.
What is the typical healing time for dental implants after they have been placed?
The initial healing period after implant surgery usually takes a few weeks. Your gums need time to close over the surgical site and reduce swelling.
The bigger wait comes from osseointegration. This process, where your bone fuses to the implant, typically takes three to six months.
Your dentist won’t attach the permanent crown until osseointegration is complete. Rushing this step increases the risk of implant failure.
Some factors can slow down your healing time. Smoking, certain medications, and health conditions like diabetes all delay the process.