Getting dental implants seems straightforward until your dentist mentions you might need a bone graft first.
Not everyone requires this additional step, but nearly half of implant patients require bone grafting to ensure implant success. Your dentist looks for specific warning signs in your jaw that signal whether you’ll need this procedure.
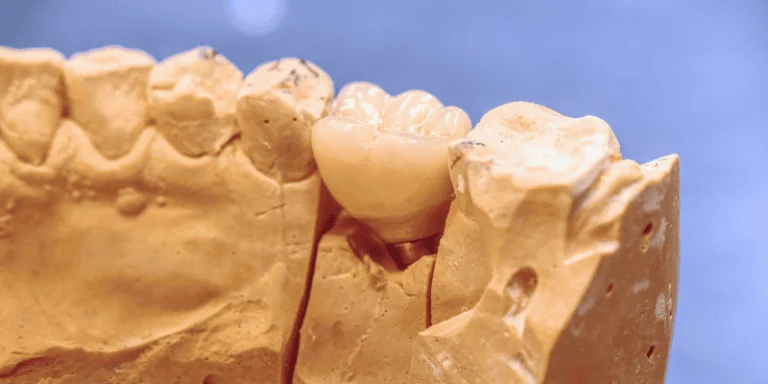
Your dentist will recommend bone grafting if your jawbone lacks the height, width, or density needed to securely hold a dental implant in place.
Several red flags alert dentists to potential problems, including how long you’ve been missing teeth, your history of gum disease, and what shows up on your imaging scans. Understanding these warning signs helps you know what to expect during your implant journey.
The good news is that bone grafting creates a strong foundation that makes implants more stable and likely to last for decades.
This guide outlines the signs you need bone grafting before implants, what happens during the grafting process, and how it sets you up for successful implants.
Key Takeaways
- Dentists look for inadequate bone height, width, or density on scans and clinical exams to determine if grafting is needed
- Common warning signs include long-term tooth loss, periodontal disease history, and narrow or shallow jawbone ridges
- Bone grafting typically requires 4 to 6 months of healing before implant placement and significantly improves long-term implant success
Understanding When Bone Grafting Is Required Before Dental Implants
Dentists evaluate specific warning signs in your jawbone before determining if you need bone grafting before dental implants. They use advanced imaging to measure bone density and volume, then assess whether your jaw can safely support an implant long-term.
Key Red Flags Dentists Look For
Your dentist checks for several warning signs that indicate you’ll need bone grafting before dental implants. Missing teeth for extended periods is a major red flag because your jawbone starts shrinking once a tooth is gone.
Periodontal disease causes bone loss around your teeth and weakens the jaw structure. If you’ve had gum disease, your dentist will carefully examine the affected areas.
Trauma or injury to your jaw can create gaps or weakened spots in the bone. Your age and certain medications also affect bone density, making your jaw less stable for implant placement.
Upper molars present unique challenges. Your dentist looks at how close your sinuses sit to your jawbone, as insufficient space requires a sinus lift procedure.
How Bone Loss Is Diagnosed Prior to Implant Placement
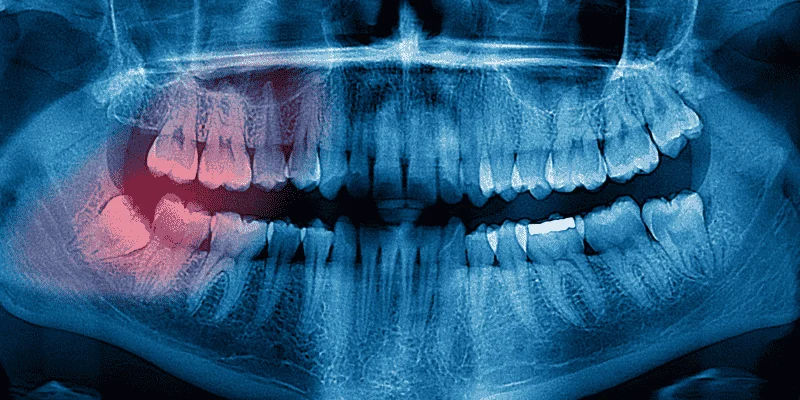
Your dentist uses CBCT scans to create detailed 3D images of your jawbone. This technology shows exactly how much bone density and bone volume you have in the area where the implant will go.
During your consultation, the dentist measures the height, width, and quality of your bone. They need at least enough bone to anchor the metal post securely and allow it to fuse properly.
3D imaging reveals hidden problems that regular X-rays miss. Your dentist can see the exact bone structure and plan the safest approach for your implant placement.
Detailed assessments help determine whether grafting is necessary for your specific situation. Not everyone needs a bone graft, but these scans give your dentist clear answers.
Risks of Skipping Bone Grafting Before Implants
If your dentist recommends a bone graft and you skip it, your implant will likely fail. The metal post won’t fuse properly with weak bone, leaving your replacement tooth unstable.
You’ll struggle to chew and speak when your implant isn’t secure. The post can shift or move, causing pain and making normal activities difficult.
Weak bone allows the implant to rub against your gums, creating inflammation and discomfort. In severe cases, the implant may pierce through your gum tissue.
Your jawbone can’t handle the chewing forces without adequate support. This leads to implant failure and means you’ll need extensive corrective surgery later. Most reputable dentists won’t place dental implants in weak bone because the complications are predictable and preventable.
Contact Minot Dental Partners in Minot, ND to schedule your bone graft evaluation and jawbone assessment with our expert team today.
Causes and Warning Signs That May Require Bone Grafting
Your jawbone needs adequate density and volume to hold dental implants securely. Bone loss from tooth extraction, gum disease, or other factors can weaken your jaw structure and make grafting necessary before implant placement.
Bone Loss After Tooth Loss
When you lose a tooth, your jawbone begins to shrink in that area. This happens because the bone no longer receives stimulation from the tooth root during chewing. Bone resorption typically starts within the first few months after tooth loss and continues over time.
The longer you wait to replace missing teeth, the more bone you lose. Your dentist can spot this on X-rays as a narrow or shortened ridge where your tooth used to be. If you’ve had missing teeth for several years, you’ll likely need a bone graft before getting implants.
Common signs of bone loss after tooth extraction:
- Visible changes in your jaw shape or facial structure
- Difficulty chewing on one side of your mouth
- Loose-fitting dentures that used to fit well
- Sunken appearance around your mouth
Effects of Gum Disease and Periodontal Disease
Gum disease is one of the most common reasons people need bone grafting before dental implants. When bacteria infect your gums, the infection can spread to the bone supporting your teeth. Advanced periodontal disease destroys bone tissue around tooth roots.
You might notice your teeth becoming loose or shifting position. This happens when the bone holding them in place deteriorates. Red, swollen, or bleeding gums are early warning signs that shouldn’t be ignored.
Even after treating gum disease, the bone damage remains. Your dentist will measure bone loss using special probes and imaging. If periodontal disease has created significant bone defects, you’ll need grafting to rebuild a stable foundation for implants.
Role of Trauma, Congenital Defects, and Osteoporosis
Physical injuries to your jaw from accidents or sports can damage bone structure. Trauma may cause immediate bone loss or create conditions where bone resorption occurs over time. Your dentist will evaluate the affected area to determine if a bone graft is needed.
Some people are born with bone defects or jaw abnormalities that affect implant placement. These congenital issues may require grafting to create enough bone volume.
Osteoporosis weakens bones throughout your body, including your jawbone. If you have this condition, your bone may be too porous or weak to support implants without grafting. Women after menopause face higher risks of bone density problems that can affect implant success.
Types of Bone Grafts and Grafting Materials Used in Dental Implants
Dentists choose from four main types of bone grafts based on your specific needs and bone loss situation. Each material has different properties that affect healing time, success rates, and what works best for your jaw.

Autografts: Your Own Natural Bone
An autograft uses your own natural bone taken from another area of your body. Your dentist typically harvests this bone from your chin, jaw, or hip area.
This approach is often called the gold standard because your body won’t reject its own tissue. Autografts contain living bone cells that promote faster healing and better integration with your existing jaw bone.
The main benefit is that autografts have superior biocompatibility and the best bone-growing properties. Your natural bone contains growth factors that help new bone form quickly around the dental implant site.
However, autografts require a second surgical site to harvest the bone material. This means more discomfort during recovery and a longer healing period. You might experience pain or complications at the donor site where bone was removed.
Allografts: Donor Bone Grafts
Allografts use donor bone from cadaver tissue that has been processed and sterilized. Tissue banks carefully screen and treat this bone material to remove any risk of disease transmission.
This type of bone graft eliminates the need for a second surgical site on your body. You’ll avoid the extra pain and healing time that comes with harvesting your own bone.
Allografts come in several forms including freeze-dried, demineralized, and cancellous bone. Each type serves different purposes based on your specific bone defect and implant needs.
The success rates for allografts are similar to autografts in most dental implant cases. The bone material acts as a scaffold that your body gradually replaces with your own bone over several months.
Xenografts and Synthetic Grafting Materials
Xenografts come from animal sources, usually cow or pig bone that has been processed to be safe for humans. These materials cost less than other options and are widely available for dental implant procedures.
Synthetic grafts include materials like calcium phosphate, hydroxyapatite, and bioactive glass. These alloplasts are made in laboratories and carry zero risk of disease transmission from human or animal sources.
Common synthetic bone materials:
- Calcium phosphate compounds
- Hydroxyapatite formulations
- Bioactive glass compositions
- Composite materials combining multiple substances
Synthetic grafts and xenografts work by providing a framework for your natural bone to grow into. They dissolve at different rates depending on the specific material your dentist chooses.
The main challenge with these bone grafting materials is that they don’t contain living cells or growth factors. This means they may take longer to integrate compared to autografts, but they avoid the need for a donor site or concerns about tissue rejection.
Don’t let weak bones hold back your smile transformation. Call Minot Dental Partner today to discuss bone grafting procedures and dental implant readiness so you can move forward confidently.
Bone Grafting Procedures for Dental Implant Success
The bone grafting procedure involves several carefully planned steps that prepare your jaw for implants. Dentists use specialized techniques like sinus lifts and ridge augmentation to rebuild bone in specific areas, while advanced imaging ensures precise placement and optimal results.
Bone Grafting Process Step-by-Step
Your dentist will first numb the treatment area with local anesthesia or offer sedation options for your comfort. They make a small incision in your gum tissue to expose the bone underneath.
The graft material is then placed into the area where bone is missing or weak. This material can come from your own body, a donor, an animal source, or synthetic compounds. Your dentist shapes the graft to fit your jaw’s natural contours.
A special membrane is often placed over the graft material. This barrier keeps soft tissue from growing into the area while new bone forms. Your dentist secures everything with small screws if needed, then closes the incision with stitches.
The entire surgical procedure typically takes 60 to 120 minutes depending on how much bone needs rebuilding. You’ll need to wait four to six months for the graft to heal before your implant surgery can proceed.
Sinus Lift and Ridge Augmentation Techniques
A sinus lift becomes necessary when you need implants in your upper back jaw area. The maxilla in this region often has insufficient bone because the sinus cavity expands after tooth loss. Your oral surgeon carefully lifts the sinus membrane and adds bone graft material underneath to create adequate height for implant placement.
Ridge augmentation addresses width or height problems along your jaw ridge. This bone grafting procedure rebuilds the ridge using block grafts or small particles of bone material. Dentists may combine this with barrier membranes to guide bone growth in the right direction.
Both techniques require precise execution. Your healing time ranges from four to nine months, but the results provide stable foundation for your implants and improve the final appearance of your replacement teeth.
Advanced Imaging and Guided Oral Surgery
Modern dentists use 3D scans like Cone Beam Computed Tomography (CBCT) to see your jaw from every angle. These detailed images show exactly how much bone you have, where it’s thin, and the precise measurements needed for your graft.
Guided surgery takes this technology further by creating a digital plan before your procedure begins. Your dentist can map out exactly where to place the graft material and plan your future implant positions at the same time. This computer-assisted approach reduces surgical time and improves accuracy.
The combination of advanced imaging and guided techniques means fewer complications and more predictable outcomes. You benefit from smaller incisions, less discomfort, and faster recovery compared to traditional methods.
Healing, Integration, and What to Expect After Bone Grafting
Your bone graft needs time to fuse with your natural jaw bone before you can get dental implants. The healing process follows specific stages that affect when your dentist can place implants and how well they work long-term.
The Healing Process and Osseointegration Timeline
Dental bone graft healing stages typically take between 3 to 6 months before your jaw is ready for dental implant placement. The first week involves inflammation and blood clot formation at the surgical site. You’ll notice swelling and discomfort during this time.
Weeks 2 through 6 bring soft callus formation, where your body builds a fibrous tissue framework. New blood vessels form to supply the healing area with nutrients needed for bone regeneration.
The hard callus phase happens between weeks 6 and 12. This is when cartilage converts to actual bone through osseointegration. Your graft material becomes fully incorporated with your existing jaw bone during this stage.
Months 3 through 6 involve bone remodeling. Your body fine-tunes the new bone structure to handle chewing forces. The timeline varies based on graft size and location, with smaller grafts healing in 3-4 months while larger reconstructions may need 6 months or more.
Post-Surgery Care for a Strong Dental Implant Foundation
The first 48 hours after surgery are critical for dental implant success. Apply ice packs for 15 minutes on and off to reduce swelling. Take your prescribed antibiotics exactly as directed to prevent infection.
Stick to soft, cool foods for at least one week. Avoid hot beverages that could dissolve blood clots. Don’t use straws, as the suction can disturb your graft site.
Oral hygiene matters for healing:
- Brush gently, avoiding the surgical area
- Use prescribed mouth rinses as directed
- Try warm salt water rinses (half teaspoon salt in 8 ounces water)
- Keep all follow-up appointments
Stop smoking completely. Tobacco use significantly reduces bone graft success rates and implant survival. Proper care creates a strong foundation for your future implants and helps maintain facial aesthetics by preventing bone loss.
Potential Risks and Complications of Bone Grafting
Most bone grafts heal without problems, but you should watch for warning signs. Contact your dentist immediately if you experience severe pain that worsens after the first week or fever above 101°F.
Red flags requiring attention:
- Excessive bleeding that doesn’t stop with pressure
- Pus or foul odor from the surgical site
- Graft material becoming exposed or falling out
- Numbness lasting beyond two weeks
Infection occurs in about 2-3% of cases. Your dentist will prescribe antibiotics if this happens. Graft rejection is rare but possible, especially with certain health conditions like uncontrolled diabetes.
Smoking increases your risk of graft failure significantly. Poor oral health can also compromise healing and affect your overall dental implant success.
In clinical studies, implants placed in grafted maxillary sinuses of smokers showed significantly lower success rates than in non-smokers, indicating that smoking increases failure risk after bone augmentation procedures.
Your dentist will monitor your progress through X-rays and clinical exams to catch any issues early.
How Bone Grafting Sets You Up for Lifelong Dental Implant Success
A proper bone graft creates a strong foundation that directly affects how well your implants hold up over the years. The time invested in healing pays off with better stability and fewer complications down the road.
Impact on Long-Term Implant Stability
Your jawbone needs enough density and volume to keep dental implants firmly in place for decades. When you get a bone graft before your dental implant treatment, you’re building the kind of support that prevents loosening or failure later on.
Without adequate bone, an implant can shift or fail within just a few years. The graft encourages new bone tissue to grow around the area, which then fuses with the implant post through a process called osseointegration. This natural bonding is what keeps your replacement tooth secure when you bite, chew, and speak.
Studies show that implants placed in grafted bone have success rates above 90% when the graft is given proper time to heal. Your bone becomes stronger over time rather than weaker, which means your implant can last 20 years or more with good care. The investment in grafting directly protects your long-term outcomes and reduces the chance you’ll need retreatment.
Dental Implant Procedure Timeline After Bone Grafting
Most people need to wait 3 to 6 months after their bone graft before the implant procedure can begin. This healing period lets new bone grow and harden enough to support the implant post.
Your dentist will use 3D scans to check bone density before moving forward. If the graft is small or your bone quality is good, you might qualify for same-day placement where the graft and implant happen during one visit.
After the implant is placed, you’ll need another 3 to 6 months for it to fuse with your jawbone. Then your permanent crown or bridge gets attached. The full process typically takes 6 to 12 months from start to finish, but this timeline ensures your implant success and prevents complications that come from rushing treatment.
Fill out the quick New Patient Form and an expert from Minot Dental Partner will connect you with an expert who can explain bone grafting, healing timelines, and implant readiness.
Frequently Asked Questions
Patients often have questions about bone grafting requirements, healing timelines, and what happens if they skip this important step. Understanding the warning signs and procedural details helps you make informed decisions about your dental implant journey.
What signs might indicate the need for a bone graft prior to receiving dental implants?
Your dentist looks for several red flags during your evaluation. X-rays that show thin or shallow bone in your jaw are the most obvious indicator.
If you’ve had missing teeth for an extended period, your jawbone may have deteriorated where the tooth roots used to be. Advanced gum disease often causes bone loss around teeth. Physical trauma to your face or jaw can damage the bone structure.
Your dentist will measure the width and height of your jawbone during your exam. If these measurements fall below the minimum needed for implant stability, you’ll likely need grafting.
How can I tell if my jawbone is strong enough to support dental implants without a graft?
You can’t determine this on your own at home. Your oral surgeon will take detailed x-rays of your jaw to assess bone quality and quantity.
During your initial exam, they’ll use these images to measure bone density and volume. The dentist checks if there’s enough healthy bone to anchor the implant securely. Not all dental implant candidates require bone grafting, so your specific situation determines the need.
Some patients have naturally strong jawbones that can support implants right away. Others need additional bone material to create a stable foundation.
What are the potential risks if I don’t get a bone graft when it’s recommended before my implant procedure?
Skipping a recommended bone graft could compromise the stability of your dental implants. Without enough bone support, your implant may fail to integrate properly with your jaw.
The implant could become loose or fall out entirely. You might experience chronic pain or discomfort in the implant area. Infection risks increase when implants don’t have adequate bone support.
Your facial structure could change over time as bone loss continues. The implant may need to be removed, requiring you to start the entire process over with bone grafting anyway.
Can you explain the various types of bone grafts available and how dentists determine the best option for me?
There are four main types of bone grafts your dentist might use. Autografts use bone taken from another part of your own body, like your hip or chin.
Allografts come from human donor tissue that’s been processed and sterilized. Xenografts use bone material from animals, typically cows. Synthetic grafts are made from man-made materials like hydroxyapatite.
Your dentist chooses based on how much bone you need and where the graft will go. They consider your overall health, the complexity of your case, and your preferences. The location of the missing tooth and the amount of bone loss also affect which type works best for you.
What should I expect during the healing process after a bone graft and before getting dental implants?
You’ll likely experience some swelling around the grafted area for the first few days. Mild discomfort is normal, and over-the-counter medications can help manage any pain.
Your dentist will give you specific instructions about caring for the graft site. You’ll need to eat soft foods and avoid anything crunchy or chewy that could disturb the area. Good oral hygiene is essential, but you’ll need to be gentle around the surgical site.
During the recovery process, you may experience some swelling around the area of the graft as well as some mild discomfort. Avoid heavy lifting or strenuous exercise during the initial healing phase.
You’ll have follow-up appointments so your dentist can check that the graft is integrating properly. These visits help ensure the new bone is fusing successfully with your existing jaw structure.
How long does it typically take for the bone graft to integrate fully before implants can be placed?
Healing times range from three to six months, depending on the complexity of the graft. The exact timeline varies based on the type of graft used and how much bone needed to be added.
Smaller grafts in areas with good blood supply tend to heal faster. Larger grafts or those in areas with less blood flow take longer to integrate fully. Your age, overall health, and whether you smoke also affect healing speed.
Your dentist will take x-rays during follow-up visits to monitor the integration process. They’ll only proceed with implant placement once they confirm the bone has healed completely and can support the implant.