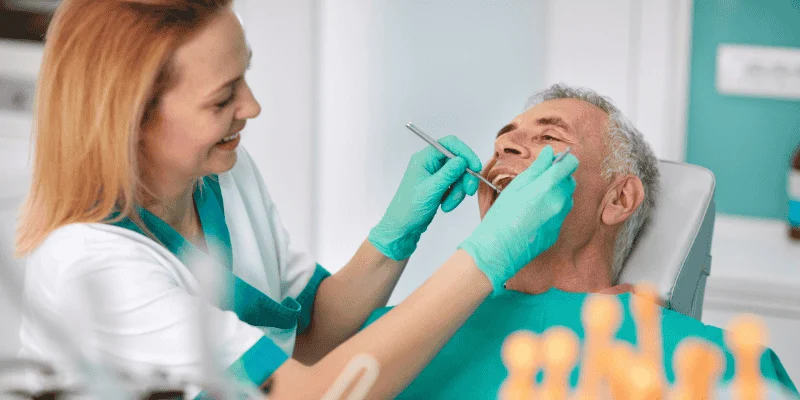
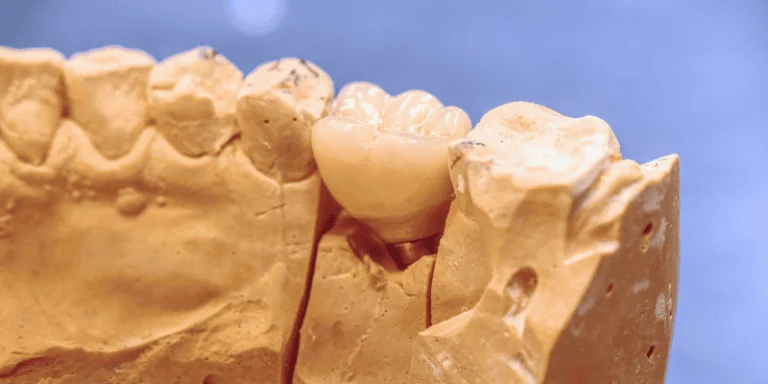
You may need closer monitoring, careful timing of surgery, and more follow-up visits when planning dental implants for diabetic patients. You can still get implants in many cases, but your dentist must adjust the plan to protect healing and lower risk.
When you have diabetes, your dentist focuses on blood sugar control, healing ability, and infection prevention to improve implant success.
High blood sugar can slow healing and raise the risk of implant failure, so your care team will review your HbA1c levels and overall health before surgery.
You may need closer monitoring, careful timing of surgery, and more follow-up visits. With the right planning and good home care, you can move forward with confidence and protect your long-term results.
Key Takeaways
- Diabetes changes how your dentist plans implant surgery and follow-up care.
- Good blood sugar control plays a key role in healing and implant success.
- Careful monitoring and strong home care help lower risks and protect your investment.
How Diabetes Influences Dental Implant Outcomes
When you have diabetes, your blood sugar levels affect how your body heals and fights infection. These changes can influence osseointegration, wound healing, inflammation, and the long-term survival of your dental implants.
Effects on Osseointegration and Bone Healing
Osseointegration means your bone grows and bonds tightly to the dental implant. This bond keeps the implant stable and allows it to function like a natural tooth root.
If you have diabetes, high blood sugar can slow bone healing. It can reduce blood flow in small vessels and affect how bone-forming cells work. This can delay or weaken osseointegration.
A large systematic review on diabetes and dental implant failure rates found that implants placed in people with diabetes had a higher risk of failure than those in people without diabetes. The risk was about 77% higher in the pooled data.
You should know that control matters. When you keep your HbA1c within target range, your implant survival rates improve. Poor control increases the chance of early dental implant failure, especially during the healing phase.
Impact on Infection Risk and Wound Healing
Diabetes can weaken your immune function. High glucose levels reduce how well white blood cells kill bacteria.
After implant surgery, your body must close the wound and protect the area from infection. If wound healing slows down, bacteria can enter the surgical site more easily. This raises the risk of early implant complications.
Research shows that well-managed diabetes has less effect on outcomes, while poorly controlled diabetes increases the chance of infection and implant problems.
You lower your risk by:
- Keeping blood sugar stable before and after surgery
- Following cleaning instructions closely
- Attending all follow-up visits
These steps support proper wound healing and protect implant survival.
Role of Inflammation and Peri-Implantitis
Diabetes often increases chronic inflammation in your body. This ongoing inflammatory state can affect the tissues around your implant.
Peri-implantitis is an inflammatory disease that damages bone and gum tissue around dental implants. It can lead to bone loss and, in severe cases, implant failure.
High blood sugar can increase inflammatory markers and make your tissues more reactive to plaque bacteria. Over time, this may raise your risk of peri-implantitis and marginal bone loss.
If you have diabetes, you need careful monitoring of your gums and bone levels. Regular professional cleanings and strong home care help control inflammation and protect long-term implant survival.
Unique Considerations for Treatment Planning
When you plan dental implants for diabetic patients, you need clear data about their health status and blood sugar control. You also need close coordination with their physician to reduce surgical risks and protect long‑term implant success.

Comprehensive Patient Assessment
You start with a detailed health history focused on diabetes mellitus, including type, duration, and current treatment. Ask if the patient has type 2 diabetes, type 1 diabetes, or is prediabetic.
Find out if they have a history of hyperglycemia, frequent infections, slow healing, or hospital visits for blood sugar issues. These details help you judge surgical risk.
Review:
- Current medications, including insulin or oral drugs
- Smoking status
- History of gum disease
- Cardiovascular or kidney complications
Long-term high blood sugar can affect bone healing and increase implant failure risk. A large systematic review on diabetes mellitus and dental implants found a higher implant failure rate in diabetic patients compared to non-diabetic patients.
You also assess oral health closely. Check for active periodontal disease, poor plaque control, and dry mouth. Treat infections before implant surgery.
If you suspect uncontrolled diabetes, delay surgery until you confirm better control.
Evaluating Glycemic Control and HbA1c Levels
You should always review recent HbA1c results before scheduling implant placement. HbA1c shows average blood sugar levels over the past two to three months.
The American Diabetes Association generally considers an HbA1c below 7% as a common target for many adults, though goals may vary by patient. Values well above this level may signal poor glycemic control.
Use this simple guide during planning:
| HbA1c Level | What It Suggests | Planning Approach |
| Below 7% | Good control | Proceed with routine precautions |
| 7–8% | Moderate control | Consider closer monitoring |
| Above 8% | Poor control | Delay surgery and coordinate care |
Patients with uncontrolled diabetes face higher risks of infection and delayed healing. Some reviews note that poorly controlled diabetes and even prediabetes can raise complication rates, including peri-implant inflammation.
You should not rely on a single reading taken months ago. Request updated labs if needed.
Medical Clearance and Interdisciplinary Collaboration
You should request medical clearance from the patient’s primary care physician or endocrinologist before surgery. This step confirms current stability and medication management.
Share details about:
- Planned surgical date
- Type of anesthesia
- Expected healing time
- Need for antibiotics
The physician can confirm whether blood sugar levels remain stable and whether medication adjustments are needed around the time of surgery.
Interdisciplinary care strengthens outcomes. The International Diabetes Federation and periodontal experts highlight the importance of coordinated management in patients with diabetes receiving implant care.
You also schedule shorter morning appointments when possible. This timing helps reduce stress and supports stable glucose levels.
Clear communication, updated lab values, and confirmed medical clearance allow you to plan implant treatment with greater safety and predictability for diabetic patients.
Surgical and Procedural Adaptations for Diabetic Patients
When you have diabetes, your dentist adjusts each step of dental implant surgery to protect healing and bone health. Careful blood sugar control, thoughtful implant planning, and precise surgical technique help lower your risk of failure and bone loss.
Pre-Surgical Protocols to Minimize Complications
Before oral surgery, your dentist reviews your recent HbA1c results and daily glucose records. Many studies show that implant outcomes improve when diabetes is well controlled, while poor control raises the risk of complications and failure, including peri-implantitis.
You may need medical clearance from your physician. Your care team may adjust insulin or other medications around the day of surgery.
Your dentist also checks for gum disease and active infection. Treating these problems first lowers bacteria levels and supports better healing.
In some cases, your provider may schedule shorter morning appointments. Blood sugar levels are often more stable earlier in the day.
Managing Bone Loss and Reduced Density
Diabetes can affect bone metabolism, especially during early healing. High blood sugar may slow bone formation and weaken your body’s defense against infection.
A large systematic review on diabetes and dental implant failure rates found that implants in diabetic patients had a higher failure risk and greater marginal bone loss than in non-diabetic patients. The difference was more noticeable in the upper jaw.
If you already have bone loss or reduced bone density, your dentist may recommend:
- Bone grafting to rebuild the jawbone
- Longer healing periods before placing the final crown
- More frequent follow-up X-rays to track bone levels
You may also need regular periodontal maintenance every 3–6 months. Close monitoring helps protect the bone around the implant.
Surgical Techniques and Implant Selection
Your surgeon may use minimally invasive techniques during dental implant surgery. Smaller incisions and careful tissue handling reduce trauma and support faster healing.
Implant design also matters. Modern surface treatments improve early bone attachment, which is important when healing may be slower.
If you need full-arch treatment, options like all-on-4 dental implants can reduce the number of implants placed and may avoid extensive bone grafting in some cases. However, careful case selection is key.
Your provider may choose:
- Implants with enhanced surface texture for better stability
- Slightly longer healing times before loading
- Staged treatment instead of immediate loading when risk is higher
Each decision focuses on protecting your jawbone and giving the implant enough time to integrate safely.
Post-Operative Care and Long-Term Maintenance
Your daily habits after surgery play a direct role in healing, implant integration, and long-term implant success. Careful cleaning, steady blood sugar control, and regular checkups lower the risk of post-surgical complications and protect peri-implant health.
Oral Hygiene Best Practices
You need consistent and gentle oral hygiene from day one. Clean teeth and implants twice a day with a soft toothbrush to protect the gum tissue around the implant restoration.
Use a low-abrasive toothpaste. Harsh products can irritate the gums and affect dental implant healing.
Add tools that reach under and around the implant crown:
- Interdental brushes sized for your spaces
- Floss or implant-specific floss
- Water flossers for hard-to-reach areas
Plaque buildup increases your risk of peri-implant inflammation. People with diabetes face a higher risk of implant failure than those without diabetes. Strong daily cleaning helps reduce that risk.
Schedule professional teeth cleanings every 3 to 6 months. Your dentist will check gum health, bone levels, and the stability of the implant restoration.
Managing Blood Sugar After Surgery
Stable blood sugar supports faster healing and lowers infection risk. High glucose levels can lead to slower healing and raise the chance of post-surgical complications.
Monitor your blood sugar closely in the first two weeks after surgery. Follow your physician’s advice about insulin or medication adjustments if your eating pattern changes.
Focus on:
- Regular meals with balanced protein and fiber
- Avoiding high-sugar snacks
- Staying hydrated
Poor glycemic control links to more implant problems. Many patients with diabetes still achieve strong outcomes when they manage their condition well.
If you notice prolonged swelling, unusual pain, or delayed tissue closure, contact your dental team right away. Early action protects implant integration.
Monitoring for Complications and Implant Success
You play an active role in tracking implant success. Watch for warning signs such as bleeding gums, bad taste, pus, or a loose implant crown.
Mild soreness is normal early on. Ongoing pain or swelling is not.
Your dentist will check:
- Implant stability
- Gum attachment around the implant
- Bone levels on X-rays
- Signs of peri-implant disease
Research shows that implants in patients with diabetes have a higher overall implant failure risk, about 77 percent higher compared to non-diabetic patients in pooled data from a large meta-analysis on marginal bone loss and implant outcomes in diabetes.
Regular follow-up helps catch small changes before they affect the implant success rate.
Keep every maintenance visit. Long-term peri-implant health depends on steady care, clear communication, and early treatment when problems appear.
Potential Complications and How to Reduce Risks
Diabetes can affect healing, infection control, and long-term implant stability. When you manage blood sugar well and follow a clear care plan, you lower the chance of serious problems.
Recognizing and Managing Infection
High blood sugar can raise your infection risk after implant surgery. It can also slow white blood cells, which your body uses to fight bacteria.
You may notice:
- Swelling that does not improve
- Red or tender gums
- Pus or bad taste
- Fever or throbbing pain
These signs need quick attention. Call your dentist right away if they appear.
You reduce risk by keeping your HbA1c in a safe range before surgery. A large review on dental implant success in patients with type 2 diabetes found that well-managed blood sugar (HbA1c below 8%) supports strong survival rates.
Brush twice a day, floss daily, and use any prescribed rinse exactly as directed. Good home care limits bacteria and protects healing tissue.
Understanding and Preventing Implant Failure
Implant failure can happen when the implant does not bond well with bone. Diabetes may cause delayed healing, which affects this bonding process.
Poor blood sugar control can reduce bone formation and slow tissue repair. This increases the chance that the implant becomes loose.
You lower this risk by:
- Checking blood sugar regularly
- Taking diabetes medication as prescribed
- Avoiding smoking
- Attending all follow-up visits
Research shows that when diabetes is controlled, implant survival is often similar to people without diabetes. Stable glucose levels before and after surgery make a clear difference in long-term success.
Addressing Peri-Implant Health Issues
Peri-implant problems affect the gum and bone around the implant. If you already have gum disease or periodontal disease, your risk increases.
Poorly controlled diabetes can lead to more inflammation and deeper pockets around implants. This condition, called peri-implantitis, can cause bone loss over time.
You protect your implant by:
- Scheduling professional cleanings every 3–6 months
- Treating gum disease before implant placement
- Monitoring bleeding when you brush
When you stay consistent with oral hygiene and medical care, you give your implant the best chance to stay healthy for years.
Benefits of Dental Implants for Diabetic Patients
If you manage your blood sugar well, dental implants can replace missing teeth stably and predictably. They support chewing, protect bone, and give you fixed tooth replacement options that fit into long-term diabetes care.
Advantages Over Dentures and Bridges
When you compare implants to dentures or bridges, stability stands out first. An implant anchors into your jawbone, so it does not shift or press on your gums the way a removable denture can.
This matters if you have diabetes. Gum tissue can heal more slowly, and loose dentures may cause sores that raise the risk of infection.
A bridge requires the dentist to grind down healthy teeth next to the gap. An implant leaves nearby teeth untouched. That protects natural enamel and lowers future dental work.
Implants also help reduce bone loss after missing teeth. Bone shrinkage can happen faster if you already face higher risk of gum disease with diabetes and dental implants. Keeping bone in place supports long-term oral health and facial shape.
Improved Quality of Life and Nutrition
Stable teeth make it easier for you to chew foods like raw vegetables, lean meats, and whole grains. These foods help you manage blood sugar.
If dentures slip, you may avoid firm or fibrous foods. That can limit protein and fiber intake. Implants stay fixed, so you can chew with more force and control.
Better chewing supports digestion and steady glucose levels. Many patients report high success when diabetes is controlled, with studies showing implant survival above 90% in controlled cases.
You may also notice clearer speech and less worry about teeth moving in social settings. That confidence can support mental well-being, which plays a role in daily diabetes care.
Tooth Replacement Options for Diabetics
You have several tooth replacement choices, even with diabetes. These include:
- Single dental implants for one missing tooth
- Implant-supported bridges for several missing teeth
- Full-arch systems such as All-on-4 for complete tooth loss
Most people with well-controlled diabetes can qualify. Dentists often look for an HbA1c below 7% and stable health before surgery.
Your dentist will review your medical history, medications, and gum health before planning treatment. With careful coordination between your physician and dental team, dental implants and diabetes can work together in a safe and structured treatment plan.
Frequently Asked Questions
If you have diabetes, you can still qualify for dental implants, but your care team will adjust the plan. Blood sugar control, gum health, and bone support all shape your results.
What are the success conditions for diabetics seeking dental implants?
You need well-controlled diabetes before surgery. Many clinicians look for an HbA1c under 7% as part of the eligibility criteria. Your dentist will also check for healthy gums, no active infections, and enough jawbone to hold the implant.
You must commit to daily oral hygiene and attend regular follow-up visits.
Smoking increases the risk of implant problems, especially if you have diabetes. If you smoke, your dentist may ask you to stop before treatment.
Can people with type 2 diabetes safely receive dental implants?
Yes, you can receive implants if you manage your type 2 diabetes well. Careful planning and steady blood sugar levels help you heal at a normal rate.
Many dentists report that patients with controlled diabetes can have outcomes similar to those without diabetes.
Your dentist may coordinate with your primary care doctor. This teamwork helps lower your risk of infection and delayed healing.
Are there any specific A1C levels required before a diabetic patient can undergo dental implant surgery?
There is no single rule for every patient, but many providers prefer an HbA1c below 7% before surgery. Some guidelines accept higher targets, up to about 8%, depending on your overall health.
If your A1C runs high, your dentist may delay surgery. You may need to improve glucose control first to reduce infection and implant failure risk.
Stable long-term control matters more than one good reading. Your recent history gives a clearer picture of how well you heal.
How can bone loss in diabetics affect the possibility of getting dental implants?
Diabetes can increase your risk of gum disease. Over time, gum disease can damage the bone that supports your teeth.
If you have lost bone, your jaw may not hold an implant securely. Your dentist will use X-rays or 3D scans to measure bone height and density.
In some cases, you may need a bone graft before implant placement. Good glucose control can help protect your remaining bone and support healing.
Is the All-on-4 dental implant procedure suitable for patients with diabetes?
You can qualify for All-on-4 if your diabetes is controlled and your general health is stable. This method places four implants to support a full arch of teeth.
Planning plays a key role in full-arch cases. Your dentist will review your A1C, gum health, and bone levels before choosing this approach. Regular maintenance visits remain essential after treatment.
What is the risk of oral implant failure in diabetic patients according to recent studies?
Implants succeed in most patients, including many with diabetes. However, poorly controlled diabetes raises the risk of infection, slow healing, and early implant failure.
Your personal risk depends on your A1C level, gum condition, smoking status, and how well you follow aftercare instructions. Good daily care and medical coordination can lower your chances of failure.