Dental implants have a success rate over 95%, but that doesn’t mean problems never happen. When something goes wrong with your implant, catching it early can make the difference between a simple fix and needing a full replacement.
The good news is that your body usually gives you clear early signs of dental implant failure before a minor issue becomes a major problem.
If you notice persistent pain, a loose implant, swelling around the gums, or difficulty chewing, these could be signs your dental implant is failing and you should contact your dentist right away.
Many people assume some discomfort is normal and wait too long to get help. But ignoring these symptoms can lead to infection, bone loss, and the need to remove the implant entirely.
Understanding what to watch for helps you protect your investment and your smile. This guide will walk you through the warning signs, explain why implants sometimes fail, and show you what steps to take if you suspect a problem.
Key Takeaways
- Watch for pain, looseness, swelling, or gum changes around your implant as these indicate possible failure
- Infections and poor bone quality are common causes of dental implant problems
- Early detection and prompt treatment can often save a failing implant before it needs replacement
Recognizing Early Warning Signs of Dental Implant Failure
Catching problems with your dental implant early can make the difference between a simple fix and losing the implant completely. Pain that won’t go away, a loose feeling, trouble eating, or movement in the implant are all signs that something isn’t right.
Persistent or Increasing Pain
Some discomfort after getting dental implants is normal during the first few weeks. But pain that continues beyond the healing period or gets worse over time signals a problem.
Sharp or throbbing pain around your implant site could mean infection or the implant isn’t bonding properly with your jawbone. You might feel this pain when you touch the area, brush your teeth, or eat.
Pay attention to pain that starts suddenly after months or years of no issues. This type of pain can indicate implant failure developing even in previously successful implants.
Don’t ignore ongoing discomfort or convince yourself it will go away on its own. Contact your dentist right away if pain lasts more than a few weeks after surgery or returns after your implant has healed.
Implant Feels Loose or Unstable
A healthy dental implant should feel just like your natural teeth. If your implant feels loose when you touch it with your tongue or finger, something is wrong.
This looseness happens when the implant hasn’t fused properly to your jawbone through a process called osseointegration. It can also mean bone loss is happening around the implant.
You might notice the implant wobbles slightly when you brush your teeth or eat. Sometimes you can feel movement that wasn’t there before. This is different from the crown on top coming loose, which is less serious than the actual implant post moving.
A loose implant needs immediate attention from your dentist. The sooner you address this issue, the better your chances of saving the implant or preventing damage to your jawbone.
Difficulty Chewing or Biting

Your dental implant should let you eat normally without any problems. Difficulty chewing or biting down comfortably can be an early sign of implant failure.
You might notice your bite feels off or different than before. Food that was easy to chew might now cause discomfort or pain. Some people avoid certain foods because chewing on the implant side has become uncomfortable.
This problem often happens when the implant hasn’t integrated properly with the bone or has started to fail. The lack of stability makes it hard for the implant to handle normal biting forces.
Watch for changes in how your teeth come together when you bite down. If the implant feels higher or lower than surrounding teeth, or if chewing causes pain, call your dentist for an evaluation.
Shifting or Movement of the Implant
A shifting implant is one of the clearest signs of failure. Your implant shouldn’t move at all once it’s healed and settled into place.
You might notice the implant has changed position slightly or tilted. Sometimes the implant crown looks different than before or no longer lines up with nearby teeth. This movement can happen gradually or suddenly.
Movement often means the bond between the implant and bone has failed or weakened. It can also indicate bone loss around the implant site. Early-stage movement may be slight, but it will worsen without treatment.
Check your implant regularly by gently pressing on it with your finger or tongue. Any movement you can detect means you need to see your dentist right away to prevent complete implant failure.
Noticing pain, swelling, or looseness around your implant? Contact our Minot, ND dental team today so we can evaluate your symptoms early and help protect your implant.
Gum and Tissue Issues Around the Implant
Your gums play a key role in keeping your dental implant secure and healthy. When the tissue around your implant starts showing signs of trouble, it often means bacteria have taken hold and inflammation has begun.
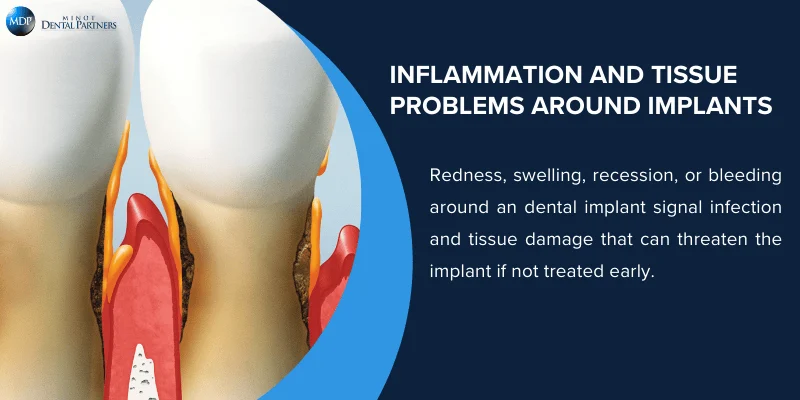
Gum Inflammation and Redness
Healthy gums around your implant should look pink and firm. If you notice redness or swelling, your body is responding to bacteria buildup near the implant site.
This inflammation often starts mild, but shouldn’t be ignored. Infection of the gums around dental implants can damage surrounding tissue when bacteria form along the abutment and below the gum line.
You might see these warning signs:
- Gums that look darker or redder than usual
- Puffy or swollen tissue around the implant
- Tenderness when you touch the area
- A feeling of warmth near the implant site
If caught early, gum inflammation can often be reversed with better oral care and professional cleaning. Waiting too long allows the problem to spread deeper into the bone.
Receding Gums and Exposed Implant
Gum recession around your implant exposes the metal post that should stay hidden beneath your gum line. This happens when inflammation destroys the soft tissue that normally covers and protects the implant.
You’ll notice the implant post becoming visible or your crown appearing longer than before. Receding gums around dental implants create pockets where bacteria can gather and multiply.
Several factors speed up gum recession:
- Poor brushing and flossing habits
- Smoking or tobacco use
- History of gum disease
- Grinding your teeth at night
The exposed implant surface becomes harder to clean and more prone to infection. Once gum tissue pulls away, it rarely grows back on its own without treatment.
Swelling or Bleeding Around the Site
Bleeding when you brush or floss around your implant isn’t normal. Bleeding during brushing or dental checkups signals that inflammation has taken hold in the surrounding tissue.
Swelling around your implant often comes with a feeling of pressure or fullness. The area might feel tender to touch or throb slightly.
Watch for these specific signs:
- Blood on your toothbrush after cleaning
- Pink-tinged saliva when you spit
- Puffy gums that feel soft instead of firm
- Fluid or pus seeping from around the implant
These symptoms mean bacteria are actively attacking the tissues supporting your implant. The longer bleeding and swelling continue, the more damage occurs to the bone underneath.
Infections and Unpleasant Sensations
Infections around dental implants create some of the most noticeable warning signs that something is wrong. A bad smell or taste in your mouth and visible discharge near the implant site signal that bacteria may be attacking the tissues supporting your implant.
Signs of Peri-Implantitis
Peri-implantitis is a serious infection that attacks the gum tissue and bone around your dental implant. This condition works similarly to gum disease but specifically targets implant sites. You might notice your gums becoming red, swollen, or tender around the implant area.
Early warning signs of dental implant trouble include bleeding when you brush or floss near the implant. The gums may also start pulling away from the implant, creating pockets where bacteria can hide and multiply.
Common symptoms include:
- Red or inflamed gum tissue
- Bleeding during cleaning
- Gum recession exposing the metal post
- Bone loss visible on X-rays
If left untreated, peri-implantitis leads to dental implant failure by destroying the bone that holds your implant in place. The infection weakens the bond between your jawbone and the implant post. You need to contact your dentist right away if you see these symptoms developing.
Persistent Bad Breath or Foul Taste
A constant bad taste or smell coming from your implant area tells you that bacteria are growing near the site. This isn’t the same as regular morning breath that goes away after brushing. The unpleasant sensation stays throughout the day, no matter how often you clean your teeth.
The foul taste often feels metallic or bitter. It comes from bacteria releasing waste products as they multiply in infected tissue. You might also notice that other people start commenting on your breath even when you’ve just brushed your teeth.
Signs of a dental implant infection shouldn’t be ignored since early treatment prevents more serious problems. The bad smell or taste usually appears alongside other symptoms like swelling or tenderness.
Your dentist can prescribe antibiotics or recommend other treatments to clear up the infection before it damages the bone supporting your implant.
Discharge or Pus Near the Implant
Pus or any fluid leaking from your gums around the implant means you have an active infection that needs immediate attention. The discharge may appear yellow, white, or greenish and often has an unpleasant smell. You might notice it when gently pressing on the gum tissue or spontaneously throughout the day.
This symptom indicates that your body is fighting bacteria around the implant site. The pus contains white blood cells, dead tissue, and bacteria. Sometimes the discharge comes with swelling that makes your face look puffy on one side.
Don’t wait to see if the problem resolves on its own. Infections that produce pus can spread quickly and destroy the bone around your implant.
Your dentist needs to clean the infected area, possibly prescribe antibiotics, and check whether the implant has loosened. Visit our clinic in Minot, ND for the best treatment and to avoid more extensive procedures.
Less Common but Serious Symptoms of Implant Problems
Some dental implant problems don’t show obvious signs like pain or swelling. Nerve damage and bone loss can develop quietly but pose major risks to your implant’s long-term success.
Numbness or Tingling in Jaw or Gums
If you feel numbness, tingling, or a burning sensation in your gums, jaw, lips, or chin, this could mean nerve damage. This happens when an implant is placed too close to a nerve or when swelling from infection puts pressure on nearby nerves.
The feeling may be constant or intermittent. You might notice it right after surgery or weeks later as complications develop.
Common areas affected by nerve symptoms:
- Lower lip and chin
- Tongue
- Gums around the implant
- Cheek on the affected side
This type of nerve involvement can affect your ability to eat, speak, and sense temperature. Don’t wait to see if it goes away on its own. Contact your dentist immediately because early treatment can prevent permanent nerve damage and may save your implant from complete failure.
Visible Bone Loss or Changes on X-ray
Bone loss around your implant is one of the most serious signs of late implant failure. You won’t see or feel this problem yourself, but your dentist can spot it during routine X-rays.
Successful osseointegration means your jawbone fuses solidly with the implant. When bone loss occurs, this fusion weakens or breaks down completely. The bone literally shrinks away from the implant threads.
Warning signs your dentist looks for:
- Dark spaces between bone and implant on X-rays
- Progressive bone loss over multiple appointments
- Bone density changes around the implant site
Bone loss often results from infection, excessive pressure on the implant, or poor oral hygiene. Without enough bone support, your implant becomes unstable and will eventually fail. Regular dental checkups with X-rays help catch this problem before it becomes irreversible.
What Causes Dental Implant Failure?
Dental implants can fail for different reasons depending on when problems occur. The quality of your jawbone and how well your implant is positioned play major roles in success, while your overall health and daily habits can also impact how well your implant heals.
Early vs. Late Implant Failure Explained
Early implant failure happens within the first few months after surgery, usually during the healing phase. This occurs when your implant doesn’t properly fuse with your jawbone through a process called osseointegration. Without this secure bond, the implant becomes loose and unstable.
Infection is the most common cause of early failure. Bacteria can enter the surgical site if you don’t keep the area clean or if contamination happens during the procedure. Poor healing due to smoking or uncontrolled diabetes can also prevent proper bone integration.
Late implant failure develops months or years after your implant has successfully healed.
This type of failure usually stems from persistent pain, swelling, or bleeding around the implant along with bone loss. Peri-implantitis, an infection similar to gum disease, is the leading cause of late implant failure and can gradually destroy the bone supporting your implant.
Role of Poor Bone Quality and Implant Placement
Your jawbone needs adequate density and volume to hold an implant securely. Poor bone quality from previous tooth loss, gum disease, or osteoporosis makes it harder for the implant to integrate. When your bone is too soft or thin, it cannot provide the stability your implant needs.
Improper implant placement during surgery creates mechanical problems. If your dentist places the implant at the wrong angle, depth, or position, it may not distribute bite forces evenly.
This puts extra stress on the implant that can cause it to loosen over time. Damage to nearby nerves or blood vessels during surgery can also interfere with healing.
Some patients need bone grafting before getting implants to build up insufficient bone.
When to Seek Help and How to Prevent Future Issues
Getting help quickly when you notice problems and following good care habits can save your dental implant. Understanding signs of dental implant failure helps you know when to contact your dentist and what steps to take.

Taking Prompt Action and Consulting Your Dentist
You should call your dentist right away if you experience any unusual symptoms around your implant. Pain that gets worse instead of better, swelling that lasts more than a few days, or any movement in your implant needs immediate attention.
Don’t wait to see if symptoms go away on their own. Early problems are usually easier to fix than issues that have been ignored for weeks or months.
Contact your dentist immediately if you notice:
- Pain that keeps getting worse
- An implant that feels loose or wiggles
- Red, swollen gums around the implant
- Pus or discharge near the implant site
- Fever or feeling sick
- Bleeding that won’t stop
Your dental team can examine the implant and take X-rays to see what’s happening beneath the gum line. Many warning signs of dental implant trouble can be treated successfully when caught early.
Preventive Care for Long-Term Implant Success
Good daily care keeps your dental implants healthy for years. Brush twice daily with a soft-bristled toothbrush, using gentle circular motions around the implant.
Floss daily around your implants using unwaxed tape or special implant floss. A water flosser can help clean hard-to-reach areas without irritating your gums.
Important preventive steps include:
- Visiting your dentist every six months for professional cleanings
- Avoiding smoking and excessive alcohol use
- Not chewing on hard foods like ice or hard candy
- Wearing a night guard if you grind your teeth
- Managing health conditions like diabetes
Proper care and maintenance significantly reduce your risk of implant problems. Tell your dentist about any medications you take or health changes, as these can affect your implants. Regular checkups let your dental team spot small issues before they become serious problems.
If something feels off with your implant, don’t wait for symptoms to worsen. Reach out to Minot Dental Partners today for expert care and peace of mind.
Frequently Asked Questions
Dental implant problems can show up in different ways at different times. Knowing what to watch for and when to get help can make the difference between saving your implant and needing a replacement.
What are the first signs that indicate my dental implant may not be working properly?
Persistent pain is often the first warning sign that something’s wrong. Some discomfort right after surgery is normal, but sharp or throbbing pain that continues for weeks or months needs attention.
A loose or wobbly implant is another clear sign of trouble. Your implant should feel stable, like a natural tooth, when you chew or brush.
Swelling and redness around the implant site may indicate infection. If you notice your gums look puffy or feel tender around the implant, don’t wait to call your dentist.
How might peri-implantitis manifest, and how does it affect dental implant stability?
Peri-implantitis is an infection around the implant that damages the surrounding gum tissue and bone. You might notice bleeding when you brush or floss around the implant area.
The gums may appear red and swollen rather than pink and healthy. Bad breath or a bad taste in your mouth that won’t go away can also signal this infection.
As peri-implantitis gets worse, it destroys the bone that holds your implant in place. This bone loss causes the implant to become loose and unstable over time. Without treatment, the implant may eventually fall out.
At which point in the healing process is a dental implant most susceptible to failure?
Early failure happens within the first 3 to 4 months after placement. During this time, your jawbone needs to fuse with the implant in a process called osseointegration.
If this fusion doesn’t happen correctly, the implant won’t be stable enough to support a crown. Poor bone quality, infection, or too much pressure on the implant can prevent proper healing.
Late failure can occur months or years after the implant seems fully healed. This type of failure often results from infection, poor oral hygiene, or grinding your teeth.
What sensations should raise concern about a potentially failing dental implant?
Ongoing pain is the most common sensation that signals problems. This pain might be constant or might only happen when you bite down or chew.
Pressure or discomfort around the implant area shouldn’t be ignored. You might also feel like the implant is shifting or moving slightly when you eat.
Increased sensitivity to hot or cold temperatures near the implant can mean trouble. If your bite feels off or different than it used to, your implant may have shifted position.
Can you visually identify a failing dental implant, and if so, what should you look for?
You can spot some signs of failure just by looking in the mirror. Gum recession around the implant may expose the metal post underneath.
The gum tissue might look red, swollen, or darker than the tissue around your natural teeth. You may also see pus or discharge coming from around the implant.
The crown on top of the implant might appear loose or tilted at an odd angle. However, bone loss often shows up on X-rays before you can see any problems with your eyes. That’s why regular dental checkups are so important.
What steps should I take if I suspect my dental implant isn’t functioning correctly?
Contact your dentist or oral surgeon right away if you notice any warning signs. Don’t wait to see if the problem goes away on its own.
Your dentist will examine the implant and likely take X-rays to check the bone around it. Early treatment often involves deep cleaning around the implant and antibiotics to fight infection.
If the implant is loose or the bone loss is severe, removal and replacement may be necessary. Your dentist might need to do a bone graft to rebuild the area before placing a new implant. The sooner you get help, the better your chances of saving the implant or successfully replacing it.