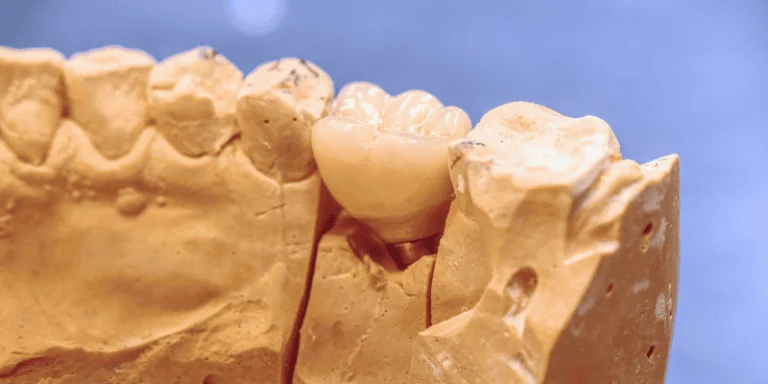
You might notice slight movement or sensitivity in a new implant during the first 90 days. This can happen while the implant fuses with your jawbone, or it may be a sign of a loose crown, infection, or too much biting force.
If the implant body itself stays firm in the bone, mild movement or soreness can be normal during healing; persistent wobbling, pain, or pus means call your dentist right away.
Keep the area clean, avoid chewing hard foods on that side, and watch for swelling or changes in how the tooth feels. Understanding why dental implants feel loose after surgery and the warning signs helps you act fast and protect the implant’s chance to heal properly.
Key Takeaways
- Mild movement or soreness can be part of normal healing during the first weeks.
- Persistent wobble, pain, or discharge needs prompt dental evaluation.
- Good oral care and avoiding hard forces help improve implant success.
Understanding Why Dental Implants May Feel Loose Early On
You may feel movement or odd sensations after implant surgery. Many causes are normal healing signs, but some problems need prompt care to protect the implant and surrounding tissue.
The Healing Process and Osseointegration
Right after your implant is placed, your body begins osseointegration, the bone growing onto the implant surface. This process takes weeks to months. Early on, the implant may feel slightly mobile while bone cells attach. That mild movement often lessens by 6–12 weeks as stability increases.
You will also have soft-tissue healing. Gums around the implant can swell, feel tender, or shift a bit. These changes can make the whole crown or temporary appear loose even when the metal post is stable.
Follow your dentist’s instructions on diet and cleaning. Avoid hard or sticky foods and don’t chew on the implant side until your clinician clears you. Good oral hygiene and avoiding smoking speed healing and reduce the chance of complications.
Differences Between Loose Implant, Abutment, and Crown
A loose feeling can come from three different parts: the crown, the abutment, or the implant post. If the crown wiggles, it’s usually a loose screw or cement and is the simplest fix. The dentist can re-tighten or re-cement the crown.
If the abutment (the small connector) moves, you might sense more wobble but still no deep pain. Abutment problems often need the dentist to remove and repair or replace it. This risks damaging the restoration, but the implant post may stay intact.
If the implant post itself is loose, that’s more serious. Loose implants often mean poor osseointegration or infection. You may get swelling, pain, or pus. If you suspect the post is loose, contact your dentist right away so they can assess and plan treatment.
Normal vs. Concerning Sensations After Surgery
Normal sensations: mild soreness, slight rocking of a temporary crown, gum tightness, and sensitivity when chewing. These usually improve in days to weeks. You might also feel pressure as bone remodels during osseointegration.
Concerning signs: increasing pain, a clear or bloody discharge that doesn’t stop, spreading swelling, fever, or a growing looseness in the implant post. If you can move the implant by hand or the abutment spins, seek immediate care.
If you’re unsure, call your dental office. Early checkups and X-rays can tell whether the implant is integrating or if infection or mechanical failure needs treatment.
If your dental implant feels loose after surgery, schedule a visit with Minot Dental Partners in Minot, ND, for a gentle exam and expert care to ensure your smile continues to heal properly.
Top Causes of Loose Dental Implants in the First 90 Days
In the first three months after surgery, looseness usually comes from either the implant not integrating with your jawbone, parts above the implant becoming loose, the implant being placed wrong, or a new injury. Each problem needs a different fix, ranging from minor tightening to redoing the implant.

Failed or Delayed Osseointegration
Osseointegration is the process where your jawbone grows onto the implant surface. If the bone does not attach firmly, the implant can move when you bite or touch it. This failure can happen because of poor bone quality, uncontrolled diabetes, smoking, or an infection at the site.
You might feel wobbling, soreness, or pain during chewing. A dentist will take X-rays and check for mobility to confirm failed osseointegration.
Treatment can include removing the implant and allowing the bone to heal, bone grafting to improve bone volume, or waiting longer if healing is simply delayed. Acting quickly lowers the risk of bone loss and further complications.
Loose Abutment or Crown Components
Sometimes the implant body is stable but the parts above it come loose. The abutment (the small connector) or the crown can unscrew, break, or wear down. This creates the feeling that the whole implant is loose even though the metal root in your jaw is fine.
Look for a crown that moves, a clicking sound, or discomfort when you bite. Your dentist can usually tighten or replace the abutment screw, re-cement the crown, or swap a damaged part. These fixes are often simple and done in one visit, but delaying care can allow bacteria to collect and cause inflammation around the implant.
Improper Implant Placement
If the implant was placed at the wrong angle, depth, or location, it may not get enough bone contact or may press on nearby structures. Poor placement can result from inadequate pre-surgical planning, not enough bone grafting, or surgical error during the implant procedure.
Problems you might notice include persistent soreness, a crown that sits too high or hits opposite teeth first, or ongoing mobility.
Treatment options vary: minor repositioning of the prosthetic parts, surgical correction, or removing the implant and placing a new one after improving the bone. Good imaging and planning before surgery reduce this risk.
Trauma or Injury to the Surgical Area
A bump, fall, or hard bite can dislodge an implant or loosen the attached crown in the early healing window. Even small trauma can interrupt osseointegration or break the abutment screw.
You may see swelling, bleeding, or sudden movement after an accident. If this happens, stop using that side to chew and contact your dentist right away. Early repair might be as simple as retightening the abutment or, if bone is damaged, removing the implant and treating the site before trying again.
Risk Factors and Conditions That Increase Looseness
Certain health problems and habits make it harder for an implant to stay stable. These issues include infections around the implant, weak or lost jawbone, and forces from grinding or a bad bite. Each one affects how well your implant bonds and how long that bond lasts.
Gum Disease and Peri-Implantitis
If you have gum disease (periodontal disease), bacteria can damage the tissues that support both natural teeth and implants. Infection around an implant is called peri-implantitis. It starts as gum redness and bleeding, then can erode the bone that holds the implant.
You might notice swelling, bad taste, or pus near the implant. These signs mean you should see your dentist right away.
Preventing peri-implantitis means keeping the area clean and getting regular professional cleanings. Your dentist can remove hardened plaque and check for early bone loss. If peri-implantitis is caught early, treatment like deep cleaning or antibiotics may save the implant.
Severe bone loss often needs more advanced care such as flap surgery or removal of the implant.
Bone Loss and Bone Quality Issues
Your implant needs healthy jawbone to fuse correctly, a process called osseointegration. If you have low bone volume or poor bone density, the implant may not integrate well and can feel loose. Past tooth infections, long-term tooth loss, or conditions like osteoporosis reduce bone quality.
Bone grafting before or during implant placement can add volume and improve stability.
After a graft, you must allow more healing time before loading the implant. Smoking and certain medications slow bone healing and raise the risk of failure. Your dentist will assess bone with X-rays and may recommend a graft or different implant size to match your jaw’s strength.
Teeth Grinding (Bruxism) and Excessive Bite Force
Grinding or clenching your teeth puts strong, repeated pressure on implants. Unlike natural teeth, implants don’t have a shock-absorbing ligament. Excessive force can loosen the abutment screw, fracture the crown, or stress the bone attachment.
You might not notice grinding during the day. Look for worn teeth, jaw soreness, or morning headaches.
Wearing a custom night guard and adjusting your bite (occlusion) can reduce harmful forces. In some cases, your dentist will use stronger implant parts, change crown shape, or add more implants to spread the load. Treating bruxism early protects your implant and the surrounding bone.
Feeling movement or discomfort around your implant can be stressful. Visit Minot Dental Partners in Minot, ND, for a quick evaluation and trusted guidance from our experienced dental team.
Warning Signs That Need Prompt Attention
Early signs include looseness, ongoing pain, and trouble chewing. Act quickly if you notice movement, swelling, bleeding, or a change in how your bite feels.

Symptoms of Implant Failure or Infection
If the implant body or the crown wiggles when you touch it or when you chew, that is a major red flag. A loose implant can mean failed osseointegration or bone loss around the fixture. Sometimes the crown or abutment is loose instead of the implant; that may be fixable without replacing the implant.
Watch for gum redness, constant bad taste, or pus near the implant. Those point to gum infection (peri-implantitis) that can erode bone fast. If you have fever or spreading swelling, call your dentist right away. Early treatment often saves the implant.
Persistent Pain, Swelling, or Bleeding
Normal soreness after surgery usually improves within a week. If pain lasts longer, gets worse, or returns months later, tell your dentist. Persistent throbbing, sharp nerve-like pain, or pain that radiates down the jaw can signal infection, nerve involvement, or bite overload.
Swollen, tender gums that bleed when you brush or floss are signs of inflammation or infection around the implant. Pus or a persistent bad taste shows an active infection. These issues raise the risk of implant failure and need prompt professional care.
Difficulty Chewing or Bite Changes
If you suddenly avoid certain foods or feel pressure when biting down, the implant or crown may be loose or misaligned. A change in how your teeth meet can overload the implant and cause micro-movement that prevents bone healing.
Grinding or clenching worsens the problem and can break the abutment or crown. If chewing feels uneven, your dentist may adjust the bite, retighten the crown, or check for bone loss. Don’t keep testing a loose implant by chewing, avoid hard foods and arrange an exam.
What To Do If Your Dental Implant Feels Loose
If your implant feels wobbly, act quickly but calmly. Check for swelling, bleeding, and whether the crown, abutment, or implant post is loose.
Immediate Steps Before Seeing Your Dentist
Rinse your mouth gently with warm salt water (1/2 teaspoon salt in 8 ounces water) to reduce bacteria and soothe soft tissue. Avoid vigorous swishing that could disturb anything still settling.
Do not chew on the side with the loose implant. Stick to soft foods like yogurt, mashed potatoes, and scrambled eggs until you see your dentist.
Use a soft-bristled toothbrush and brush twice a day around the implant site, but be gentle for now. Floss carefully on the other teeth to avoid shifting pressure.
Call your dental office right away and describe whether the crown moves, the abutment feels loose, or the whole implant is unstable. Ask for an appointment within 24–48 hours and follow any specific instructions they give.
Why You Should Not Attempt Home Fixes
Do not tighten screws, glue the crown, or push the implant with your fingers. Home repairs can damage the implant, abutment, or surrounding bone.
Avoid OTC dental cement or superglue; these substances can trap bacteria and make professional repairs harder. They may also contaminate impressions or X-rays your implant specialist needs.
If pain or swelling grows, do not wait. Over-the-counter pain relievers can help, but they don’t treat the cause. Trying to “fix” the implant at home often turns a minor problem into a major one that requires removal.
When to Contact a Dental Implant Specialist
Contact a dental implant specialist or your dentist if the implant feels loose for more than a few hours, if you have increased pain, pus, or spreading swelling. These signs can mean infection or bone loss.
If the crown or abutment is loose but the implant post seems stable, the specialist may be able to tighten or replace parts without removing the implant. If the post is loose, you’ll need evaluation and likely removal.
Bring any notes about when the implant was placed, recent injuries, and your home care routine (including if you brush twice a day with a soft-bristled toothbrush). This helps the specialist plan X-rays and a quick treatment during your visit.
Do not ignore early warning signs. Call Minot Dental Partners for prompt implant support and compassionate care designed to prevent complications and restore your comfort.
Prevention and Aftercare for Secure Dental Implants
Keep the implant area clean, protect the crown from hard forces, and follow your dentist’s checkup schedule. Small daily habits and timely visits prevent infection, bone loss, and most early loosening.
Maintaining Good Oral Hygiene Habits
Brush twice a day with a soft-bristled toothbrush and use low-abrasive toothpaste to avoid scratching the crown or abutment. Angle the brush at 45 degrees to the gumline and clean gently around the implant for 2 minutes each session.
Floss once daily using implant-friendly tools: waxed floss, a floss threader, or a water flosser to remove plaque where the gum meets the implant. Focus on the sides and under the crown margin.
Rinse once a day with an antimicrobial mouthwash if your dentist recommends it. Avoid vigorous rinsing in the first week after dental implant surgery. If you notice bleeding, persistent bad taste, or increased soreness, call your dentist right away.
Attending Follow-Up Visits and Checkups
Attend all scheduled follow-up visits after dental implant surgery. Your dentist will check osseointegration, tighten the abutment if needed, and take X-rays to watch bone levels. Early visits usually fall at 1–2 weeks, 6–8 weeks, and around 3 months, but follow your provider’s exact plan.
Bring a list of any changes you feel, movement, new pain, or pus. Your dentist can treat mechanical issues (like a loose crown) quickly or start care for infection before bone loss occurs. Regular maintenance visits every 6–12 months help keep implants stable long-term.
Protecting Implants from Excessive Forces
Avoid hard foods like ice, hard candy, and unpopped popcorn kernels that can crack crowns or loosen screws. Cut tough foods into small pieces and chew on the opposite side while healing.
If you grind or clench your teeth, ask for a custom night guard. A guard spreads pressure and reduces micromovement that can harm osseointegration. Sports also pose risk, use a mouthguard for contact activities.
If you experience a blow to the mouth or sudden mobility, contact your dentist immediately. Quick action can often save an implant or the prosthetic components.
Have concerns about your recovery timeline or implant stability. Reach out and let our team help you heal with confidence.
Frequently Asked Questions
You will find clear answers about symptoms, risks, causes, and fixes for a loose dental implant in the first 90 days. Read each short answer to know when to call your dentist and what to expect next.
What are the symptoms of a loose dental implant crown?
You may feel wobbling when you bite or touch the tooth.
The crown might shift, rock, or make a clicking sound when you chew.
You could notice food catching around the crown or the crown sitting higher or lower than nearby teeth.
Pain is not always present, but increased sensitivity or soreness can occur.
Should I consider a loose dental implant an emergency situation?
If you feel strong pain, swelling, pus, or a fever, seek care right away.
Those signs can mean infection and need prompt treatment.
If the crown simply feels wobbly without pain, call your dentist for an appointment within a few days.
Avoid chewing on that side and do not try to tighten or remove the crown yourself.
What could cause a dental implant to start moving slightly?
A loose crown often comes from the crown or abutment loosening.
Sticky foods, biting hard objects, or a recent face injury can dislodge the crown or screw.
In the first 90 days, poor healing or lack of bone integration can let the implant shift.
Infection, aggressive clenching or grinding, and surgical errors also increase the risk.
Can anything be done to fix a loose implant tooth?
Yes. If the crown is loose, the dentist can re-cement or retighten the crown or screw.
If the abutment is loose, the dentist can replace or repair that piece.
If the implant post has failed to integrate or is infected, the dentist may remove it and treat the area.
After healing, you can often receive a new implant or alternative restoration.
At what point do dental implants typically start to feel normal?
Most people start feeling stable by three months as the implant fuses to bone.
Full integration usually takes 3–6 months, depending on health and bone quality.
If you still feel movement after three months, tell your dentist so they can check healing and bite forces.
Delays may come from infection, bone issues, or habits like grinding teeth.
Is there a procedure to tighten a loose dental implant?
If the crown screw is loose, your dentist can access and tighten it during a short visit.
A loose crown may be re-cemented or replaced on the spot.
If the implant post is loose because it never integrated, your dentist may remove it and plan for a staged replacement after healing.
Treating infection and rebuilding bone are common steps before reimplantation.