Dental implant therapy is growing rapidly in the U.S., driven by an aging population and higher tooth retention.
National surveys indicate that implant prevalence has risen from 0.7% (U.S. adults, 1999–2000) to 5.7% (2015–2016), with projections reaching ~20–23% by 2026. This surge makes implant longevity, typically measured by 5-, 10-, and 20-year survival rates, a key concern.
Contemporary research consistently reports high dental implant success rates in North Dakota and other states in the U.S.
For example, a 2008 meta-analysis reported an overall 5-year implant survival of ~96.8% (implant-supported single crowns), whereas a 2019 review reported a 10-year survival of ~96.4%.
A 2024 meta-analysis of 20-year studies reported survival rates ranging from ~88% to ~92% (short-term prospective vs. longer-term retrospective data), indicating roughly 4–5 out of 5 implants in the last two decades.
In summary, national implant survival is very high (≈95–97% at 5 years, ≈93–97% at 10 years, and ~80–90% at 20 years).
Traditional vs. Mini Implants
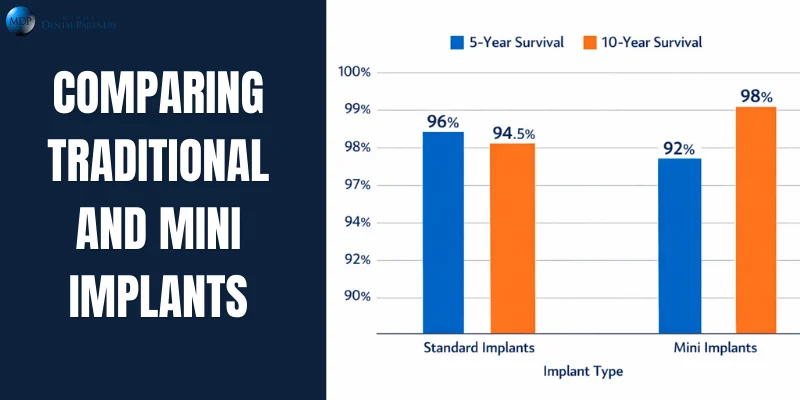
Dental implants are broadly categorized by size. Standard (conventional) implants typically exceed 3.0 mm in diameter and are used to support single crowns, bridges, or overdentures. Mini (narrow-diameter) implants (<3.0 mm) are often used for denture stabilization in narrow ridges or medically compromised patients.
The longevity profiles differ somewhat: mini implants have shown somewhat lower midterm survival in some studies, but can perform equivalently in favorable cases.
For mandibular overdentures, one study reported a 15-year mini-implant survival of 97.9%, comparable to conventional implants. A systematic review of overdentures reported a mean survival of ~92.3% for mini-implants (mean 2.5-year follow-up).
By contrast, conventional implants for overdentures or crowns routinely show ≥95% survival at 5–10 years. Notably, mini implants tend to fail more often in the maxilla (reported 31.7% failures) than the mandible (4.9% failures), likely due to poorer bone quality.
Clinicians thus view mini implants as a valid alternative when standard implants are contraindicated, but recognize a slightly higher early failure risk, especially in the upper jaw.
| Implant Type | Typical 5-yr Survival | Typical 10-yr Survival | Notes |
| Standard implants | ~95–97% | ~93–96% | High long-term success; suitable for most cases. |
| Mini implants | ~92% (overdentures) | ~98% (mandibular) | Useful in narrow ridges; higher failure if placed in the maxilla. |
Regardless of type, revision/re-treatment remains relatively rare. Large cohort data suggest implant failure rates of only ~2–5% over 5–10 years. For example, a Chinese cohort found a 2.4% implant-level failure over ~3 years.
When implants fail, replacing them (reimplantation) generally succeeds: reinserted implants have ~95% survival over ~3 years. Meta-analyses of reimplantation report survival rates of ~90–95% for replacement implants. Thus, most failures can be managed with high success by re-treatment.
Find out your personal dental implant success outlook. Schedule a consultation with Mintor Dental Partners today at Minor, ND, clinic.
Contributing Factors to Longevity
Multiple factors influence implant outcomes in all regions. Patient systemic health and behaviors are key: smoking roughly doubles implant failure risk, and head/neck radiotherapy also doubles risk.

Chronic diseases (e.g., poorly controlled diabetes, osteoporosis) have shown weaker or inconsistent effects on implant failure in pooled studies, but may still complicate healing in practice.
Good oral hygiene and maintenance are crucial for preventing peri-implantitis; poor plaque control is a primary risk factor for bone loss around implants. In short, a smoker or patient with untreated periodontal disease faces higher late-failure rates.
Surgical and biomechanical factors also matter. Adequate bone volume, optimal implant positioning (avoiding vital structures) and surgical technique (flap vs. flapless, immediate vs. delayed placement) affect success. Roughened implant surfaces and longer lengths improve osseointegration, especially in softer bone.
Immediate or early loading can increase early failures if conditions are unfavorable.
Prosthetic design is also influential: overcontoured crowns, cement remnants, or unfavorable occlusion can contribute to complications. A recent review notes that prosthetic factors, crown contours, abutment design, and occlusal scheme, significantly affect peri-implant health.
For example, poorly fitting prostheses or excessive bite forces can lead to screw loosening or fracture. Material choice has a minor impact: current evidence suggests zirconia (ceramic) implants have similar short-term survival as titanium, though some trials hint at slightly lower survival for one-piece zirconia vs. titanium.
In summary, implant longevity is maximized when patient risk factors are managed (e.g. smoking cessation, disease control), surgical planning is meticulous, and prosthetic work is well-designed and maintained.
Want long-lasting dental implants backed by proven outcomes? Talk with the team at Mintor Dental Partners.
National Trends and Projections
In the past five years (2019–2024), the use of dental implants and associated technologies has continued to expand. Utilization is rising most among older adults: NHANES analysis (1999–2020) shows implant prevalence in U.S. adults 50+ jumped from 1.3% to 8.4%.
The implant market is growing steadily (projected ~5.8% annual growth) with a U.S. market ~$2.3 billion by 2034. Demographically, older Americans will greatly increase demand: by 2030 U.S. seniors will outnumber children, boosting needs for prosthetic tooth replacement.
National data still show substantial tooth loss despite improvements. About 20% of U.S. adults 65+ have no natural teeth, and ~44% have lost ≥6 teeth.
Even as edentulism declines (e.g. only ~10–11% of U.S. seniors fully edentulous by 2022【47†】), partial tooth loss remains widespread (≈120 million Americans missing ≥1 tooth, 36 million completely edentulous).
These gaps translate into rising demand for implants. Analyses indicate implants will become increasingly mainstream for middle-aged patients; by the mid-2020s a sizable minority of adults will have implants.
Continuing advancement, digital planning, novel materials, mini-implant systems, should further improve outcomes, though no major decline in survival is expected. Importantly, experts emphasize the need for lifelong monitoring beyond the first decade as more implants remain in place for decades.
North Dakota Context
North Dakota (ND) lags behind national averages in oral health and dental care access, which may influence implant demand and outcomes. ND has historically had higher tooth-loss rates: a 2016 survey found ~31.8% of ND nursing-home seniors were edentulous (vs. ~15–20% U.S. seniors). However, ND’s oral health is improving.
Recent behavioral surveillance shows a steep decline in senior edentulism: from ~25% of ND seniors in 2004 down to ~12–13% by 2020【47†】, nearly closing the gap with national levels. Similarly, ND residents with extensive tooth loss (missing ≥6 teeth) fell from ~49% (2004) to ~30% (2022), though still slightly above the U.S. (~25–27%).
These trends reflect better prevention and dental care in ND, aided by state programs and fluoridation.
Despite improvements, ND has notable access barriers. Many rural areas face shortages of dentists, with one analysis showing rural ND ratios of approximately 1:2,400 residents (urban ~1:1,500). Over 60% of ND’s dentists practice in cities like Fargo, Bismarck, and Minot.
As a result, rural patients often travel far for advanced care. ND also generally lacks comprehensive dental insurance coverage: for example, ND Medicaid explicitly excludes implants for adult beneficiaries, limiting access for low-income seniors who might need them.
These factors indicate that, although statewide implant success rates should parallel national figures (given similar implant systems and surgical standards), the number of implants placed per capita in ND may be lower due to access barriers.
On the outcomes side, no published data specific to ND implant survival were found. In the absence of local studies, one assumes ND surgeons achieve similar success rates to their peers. ND oral health reports focus on prevention and general status; neither the Department of Health nor local organizations report implant-specific metrics.
Thus, comparisons rely on national data and on extrapolating ND tooth-loss trends. Overall, ND’s aging population and high historic tooth loss imply growing future implant demand. The state’s improvements in tooth retention (Figure below) suggest many eligible seniors will opt for implants rather than dentures, assuming they can find providers.
Figure: Tooth loss trends in Minot/Ward County, ND. Ward County (Minot) has a relatively young, affluent population with slightly lower reported tooth loss than statewide averages (12.4% adults ever had a permanent tooth extracted vs. 13.5% ND).
This suggests Minot residents may have somewhat better dental health and access than rural areas.
Considering implants but unsure about success rates? Talk to an expert at the Mintor Dental Partners for expert advice.
Minot (Ward County) Local Insights

Minot (Ward County) is ND’s principal urban center in a largely rural region. Its demographics and oral health differ from rural ND. The population is younger and wealthier: only ~12% are 65+ (vs 15% ND), and median household income (~$64K) exceeds the ND average.
Ward County’s poverty rate (8.4%) is lower than the state’s (11.0%), and elderly poverty is also lower (5.8% vs 8.0% ND). These factors correlate with better dental health. Indeed, the Ward County health profile (2019) notes only 12.4% of adults reported ever having a tooth extracted, roughly on par with (or slightly better than) the ND average.
No published data exist for implant usage or outcomes specifically in Minot. However, given Minot’s urban status, residents likely have higher dental utilization than remote ND areas.
Minot has several general and restorative dental practices (including at least one implant specialist center), so local patients can access implant services more readily than in smaller towns.
Still, specialized care (e.g. complex bone grafting) may require travel to larger cities. In short, Minot’s younger, insured demographic and better access suggest its implant success rates should meet or exceed ND averages, but no formal reports are available.
Local dental practices do emphasize implants (e.g. marketing on recovery and technology), yet objective clinical data (surveys or registry) for Minot are lacking.
Trends and Projections Beyond 2026

Looking forward, implant dentistry continues evolving. The U.S. patient population that might benefit from implants is aging: by 2029, one in four North Dakotans (23 counties) will be 65+, mirroring national aging. With more patients retaining teeth into old age, many will need implant rehabilitation for tooth loss.
Market analyses project steady growth: U.S. implant market revenue is expected to rise ~5–6% annually into the 2030s.
Technological trends, digital imaging, 3D printing, novel implant surfaces and materials, promise incremental improvements but have not dramatically changed survival statistics. If implant adoption hits ~20% of adults by 2026 and continues upward, the overall number of implants placed (and thus re-treatments over time) will rise.
Experts emphasize that long-term follow-up must become standard, since implants placed today will increasingly remain in situ for 20–30 years or more. For the U.S. as a whole, no data sources currently project a decline in implant survival; in fact, ongoing research on risk mitigation may further reduce failure rates.
In North Dakota and Minot specifically, trends mirror the national picture. ND’s improving dental health and aging will increase implant demand; one analysis notes ND seniors lost fewer teeth over the 2010s【47†】, suggesting rising numbers will become candidates for implants rather than dentures.
However, ND’s rural access challenges will persist unless policy changes occur (e.g. expanded Medicaid dental benefits or rural provider incentives).
If access improves, ND could see a sharp rise in implant placements among older adults. Conversely, if workforce shortages persist, treatment delays may limit uptake.
No formal projections for ND or Minot implant trends were found; however, given national demographics and the state’s high historical edentulism, local demand is likely to grow. The image below (Figure) contextualizes Minot’s advantage in demographics and access.
Ready to explore long-lasting tooth replacement options with proven success rates? Visit Mintor Dental Partners and meet our specialists for a full implant evaluation and treatment plan.
Summary
Nationally, dental implants have very high longevity: ~96–97% survive at 5 years and ~93–96% at 10 years. Even at 20 years, success rates remain strong (~80–90%). Mini implants perform slightly lower on average (~92% midterm survival in overdenture cases) but can achieve nearly equivalent long-term survival in suitable situations.
Implant failure rates are generally low (a few percent per 5–10 years), and re-treatment (re-implantation) is usually successful (~90–95% survival). Key factors that enhance longevity include controlling systemic risks (e.g. smoking cessation), optimizing surgical technique and implant design, and ensuring well-fitting prosthetics with good hygiene maintenance.
In North Dakota, patients currently achieve implant outcomes similar to the national norm (given similar clinical practices), but the state’s high rural population and lack of public coverage may limit implant utilization.
ND has made progress in reducing tooth loss [47†], but older adults still have higher edentulism rates than much of the U.S., indicating significant unmet need. Minot/Ward County stands out as younger and wealthier, likely with better access and oral health than rural ND (Figure).
While no local implant data exist, one would expect Minot’s outcomes to match or exceed state averages, given its demographics and concentrated dental workforce.
Projections beyond 2026 are optimistic: implant technology continues to improve and dental public awareness is high. As the population ages and more teeth are retained, demand for implants will likely increase. Provided clinicians maintain high standards of planning and follow-up, implant longevity should remain excellent.
Ongoing research into materials (e.g. comparing titanium vs. ceramic implants) and techniques (e.g. digital workflows) may further refine outcomes. In sum, dental implants offer a predictable, long-lasting solution for adult tooth loss, with success rates that far exceed most other restorative options.
By monitoring risk factors and promoting preventive care, practitioners and policymakers can help ensure that Americans,from Anchorage to Atlantic to Minot, reap the full benefits of implant dentistry.
Data Sources
| Statistics | Source | Report/Study Title |
| Implant prevalence rose 0.7% → 5.7% (1999–2016) | PubMed / Journal of Dental Research | Trends in Dental Implant Use in the U.S., 1999–2016 (PubMed) |
| Same prevalence statistic confirmation | International Dental Journal (UCL repository) | Income or Education: Association With Dental Implant Use (UCL Discovery) |
| Implant success ≈ 90–95% over 10 years | U.S. National Library of Medicine (PMC) | Clinical review of implant survival (NCBI) |
| Implant success 90–95% overall | Cleveland Clinic | Dental Implant Surgery Overview (PubMed) |
| 120 million Americans missing ≥1 tooth | American Dental Association | Dentures Topic Page (Ada Association) |
| Same tooth-loss statistic | University of Alabama at Birmingham | Prosthodontics news article (University of Alabama at Birmingham) |
| 36 million Americans edentulous | American College of Prosthodontists | Missing Teeth Fact Sheet (American College of Prosthodontists) |
| Edentulism prevalence 13.7% in U.S. adults 65–74 | PubMed Central | Periodontitis prevalence in adults ≥65 (PMC) |
| ND seniors tooth loss charts | North Dakota Dept. of Health | Older Adult Oral Health Report (Health and Human Services North Dakota) |
| ND older adult edentulism data (BRFSS) | North Dakota State Plan | Oral Health State Plan (North Dakota Legislative Branch) |
| 31.8% long-term-care seniors edentulous (ND) | Regional ND dental report | ND implant trends article summary (Minot Dental Partners) |
| Rural dental access disparity | Harvard Gazette | New study maps the dental deserts in the U.S. (Harvard Gazette) |
| Rural dentist shortage | University of North Dakota | Educating the Oral Healthcare Workforce in North Dakota (Center for Rural Health) |
| U.S. dentist ratio ≈ 61 per 100k population | American Dental Association (HPI) | Dentist Workforce – Key Facts (Ada Association) |